 In recent years, supplementing vitamin D3 has been touted as somewhat of a cure-all, but is that really the case?
In recent years, supplementing vitamin D3 has been touted as somewhat of a cure-all, but is that really the case?
According to the New York Times, "Millions of people are popping supplements in the belief that vitamin D can help turn back depression, fatigue, muscle weakness, even heart disease or cancer. In fact, there has never been widely accepted evidence that vitamin D is helpful in preventing or treating any of those conditions."
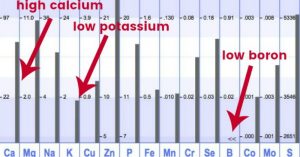
Vitamin D3 advocates always share the benefits, but they rarely talk about what can happen when you take too much. Vitamin D supplementation has a drastic effect on your mineral levels, namely calcium, potassium and boron which drastically alters your metabolic rate. Unfortunately this is something that is rarely talked about or acknowledged.
Yet it's taken daily in vitamin D supplements, multivitamins, and other combination supplements. Often it's taken in multiple different supplements at the same time, something I call "supplement stacking."
Just like all other dietary trends, the truth surfaces eventually... and surprise-surprise that truth is that a pill or supplement is NEVER the cure-all you're led to believe. If low vitamin D doesn't mean you just need to supplement vitamin D, what does it mean?
What low vitamin D can REALLY reveal
It appears that low vitamin D levels are the result of ill-health, but not the cause. Low vitamin D levels can reveal a host of things:
- Ill-health: According to a recent study done in December 2013 in Lancet Diabetes & Endocrinology, "The discrepancy between observational and interventional studies suggests that low 25(OH)D is a marker of ill health."
Additionally, a 2014 study looked at the link between inflammation as a cause of low vitamin D, "Despite increased supplementation chronic inflammatory diseases are on the rise. Attention to the alternate hypothesis-low 25(OH)D is a consequence of the chronic disease process, provoked by persistent intracellular infection-may be crucial to reversing this trend and needs further research. The prevailing dogma that the level of serum 25(OH)D provides an accurate assessment of vitamin D status needs closer examination. Circulating levels of 25(OH)D may not be an accurate reflection of vitamin D status. In those with an autoimmune disease or chronic inflammatory symptoms, 1,25(OH)2D may be elevated."[6, 11] - Low calcium intake: Chris Masterjohn explains that vitamin D levels and calcium levels go hand in hand. "Overall, then, we would expect that a deficiency in calcium would cause low 25(OH)D, and that correcting the deficiency would normalize the 25(OH)D, but that beyond a certain threshold, increasing calcium intake might not increase 25(OH)D any further." [4] Additionally, he adds, "As a rule of thumb, then, I would say that if someone has low 25(OH)D and she is eating two to three servings of dairy products or soft, edible bones, or two to three cups of cruciferous vegetables per day (which have their downsides), then calcium deficiency is unlikely to be the explanation. If one is not eating these foods, however, it could very easily be the explanation. In such a case, the person has little to lose and much to gain by including more calcium-rich foods." [4]
- Poor digestion: Low vitamin D status can also be a reflector of poor gut health, especially since proper digestion is a precursor to good health. You can't be healthy without good digestion to make nutrients available and absorbable by the body. Digestion is king when it comes to health, and there are a host of reasons why people have poor digestion. The ones I see most frequently are due to a slowed metabolism, low nutrient diet, and chronic stress.
- Low magnesium intake: "Intake of magnesium significantly interacted with intake of vitamin D in relation to risk of both vitamin D deficiency and insufficiency." [7] And "Magnesium deficiency shuts down the vitamin D synthesis and metabolism pathway." As well as, "A randomized trial indicates that magnesium optimizes vitamin D status, raising it in people with deficient levels and lowering it in people with high levels." [12]
- Glyphosate (ie. Roundup, GMOs, non-organic food): This herbicide disrupts the key class of liver Cyp enzymes that are key for detoxifying chemicals as well as essential for activating vitamin D. Meaning, it could be vitamin D levels are low because the liver can't activate the vitamin D because of how the glyphosate is disrupting the enzymes that are essential to the process. [13]
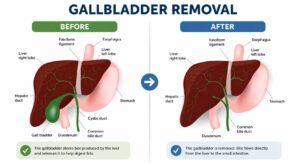
- Malnourished liver: Liver health plays a role in the absorption of vitamin D, because it affects both the production and flow of bile. Bile emulsifies fat (vitamin D is a fat soluble vitamin), and makes it more available for absorption in the gut.
- Boron deficiency: the mineral boron beneficially impacts the body's use of estrogen, testosterone, and vitamin D [14]
- Vitamin C deficiency: vitamin D deficiency is less likely when one has optimal levels of vitamin C [15]
https://youtube.com/watch?v=XRoNIOYpFLg%3Fsi%3DlMTAjc7ipvMsLEIk
Vitamin D supplements - a magic bullet that may not be so magic?
As you may see, taking a vitamin D can sometimes be a distraction because it does not address the root cause of low vitamin D levels; a host of other issues contributing to ill-health.
However you slice it, vitamin D is still a hormone, and supplementation should be done carefully after proper testing since overdosing does pose risks.
According to Chris Masterjohn, "Vitamin D can be a double-edged sword: adequate vitamin D prevents heart disease, but too much vitamin D promotes heart disease. The available evidence suggests that the lowest risk of heart disease occurs when vitamin D status is between 20 and 40 ng/mL." [5]
Vitamin D Supplement Side Effects
Two major side effects of vitamin D is that it raises your calcium levels while driving down potassium levels. The impact of this on how you feel is highly significant. It can literally make your metabolic rate slower, since according to the fundamentals of hair analysis, the calcium to potassium ratio shows how well your thyroid hormones are doing their job. This is a pattern that I see with about 90% of my hair analysis clients who take high dose vitamin D supplements regularly.
Naturopathic Doctor Garret Smith warns, "Taking calcium and/or Vitamin D will provide a push to absorb more calcium from the gut and also to raise calcium levels in the blood, this is what these nutrients do and makes sense. The question becomes, when that calcium goes up higher than desirable in the blood, how does the body compensate for it? I'm going to tell you that it transfers it into "savings accounts" to clear it from the blood that you really won't like…calcium deposits in the joints (aka osteoarthritis), kidneys (stones), blood vessels (heart disease), and even the brain." [10]
https://youtube.com/watch?v=IHsd4KYdKYU%3Fsi%3Dp5Lvg9axuvUBszOy
Here are some more side effects you may want to be aware of as well...
- Excessive Vitamin D May Increase the Risk of Autism in Infants
- Vitamin D Can Be Immunosuppressive
- Hypercalcemia and Metastatic Calcification
- Vitamin D May Cause Brain Lesions in the Elderly
Bottom line
I always question supplement trends, especially anything marketed as a "cure-all" or "easy button."
Instead of taking the "easy" path of trying to resolve a vitamin D deficiency with vitamin D supplements, I'd rather address the root cause(s) of low vitamin D levels first: nutrition? gut health? vitamin or mineral status? poor sun exposure?
Sometimes just asking yourself, "why do I have low vitamin D levels" versus just buying a supplement enables you to look at the situation from a whole new angle and address important vitamin and mineral levels that impact vitamin D levels (hint: vitamin C, boron levels, magnesium levels).
These things would be totally ignored or missed if you just popped a supplement that you might not even need (why testing is so important).
That's where the true magic happens, when you learn to think about your body in a whole different way. Good nutrition isn't about just picking up a supplement, it's about diving deeper, understanding your body, and getting strategic with what your body needs.
Some vitamin D is good. More is not always better. Testing before taking high dosages is smart.
Want to see how your vitamin D supplementation is impacting your thyroid and mineral levels?
With a simple hair analysis test, you can discover if vitamin D supplements are having an ill-impact on your mineral levels, your metabolism and your health. Read all about why else you'd want to cut off your hair for your health here or enter your email below to learn all about the best way to understand your own mineral levels with hair analysis.
Get started with hair analysis.
Do you have low vitamin D levels? Please share in the comments what you think!
PIN IT:
References:
1. http://www.ncbi.nlm.nih.gov/pubmed/23126292
2. http://180radio.com/180degreehealth-8-dont-supplement-vitamin-d-youre-heard/
3. https://www.facebook.com/DrGarrettSmith/posts/675817219163593
4. http://web.archive.org/web/20160819000355/http://www.westonaprice.org/our-blogs/cmasterjohn/an-ancestral-perspective-on-vitamin-d-status-part-2-why-low-25ohd-could-indicate-a-deficiency-of-calcium-instead-of-vitamin-d/
5. http://www.westonaprice.org/modern-diseases/beyond-cholesterol/
6. http://www.thelancet.com/journals/landia/article/PIIS2213-8587(13)70165-7/abstract
7. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3765911/
8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3854088/
9. https://www.facebook.com/DrGarrettSmith/posts/645526842192631
10. http://www.weedemandreap.com/hair-mineral-analysis/
11. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4160567/ add
12. https://www.sciencedaily.com/releases/2018/12/181214093837.htm
13. https://myersdetox.com/transcript-166-glyphosate-and-how-to-detox-it-with-dr-stephanie-seneff/
14. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4712861/
15. https://www.ncbi.nlm.nih.gov/pubmed/2170601




Allyson Turner says
I'm so glad to hear you say this. I was suspect about the Vitamin D craze from the get go. Especially, since it's supposed to be the "sunshine vitamin". I mean, how is it possible to bottle up the sun? Exactly.
As usual Catherine, great reporting. Thanks for keeping your finger on the pulse!
Frank Havnoonian says
Allyson-
Sunlight has a wide array of wavelengths. It is the UV part of the electromagnetic spectrum that effects the cholesterol in our skin converting the cholesterol into a form of Vitamin D. And we must stop calling it a vitamin. It is a pre-steroidal hormone and from an evolutionary biology point of view the oldest hormone in our body as it predates testosterone and similar hormones. by a million years....... 2,000 years ago we did 2 things that todays life style has no understanding of. We ate more fish AND lived outside.. Fish eat the photoplankton sitting near the top of the water and we eat the fish...So very few were deficient. Different problem today. Many drs today worry that our children don't exercise outside ...They are Inside playing video games which will lead to a shorter lifespan.. When I was diagnosed with extremely low vitamin D 7 years ago they gave me a once-a-week megadose of 50,000 IUs of "D" and after the third of 6 pills...I was a different person. So many maladies /illnesses went away that as a former scientist - its power to cure left me in awe of the importance of sunshine vitamin .
Michelle says
I agree. I was taking 114,000 IUs prescribed by doctor and could not believe how much better I felt after 2 weeks on the Vitamin D.
Carrie C says
Michelle, while it is "called' the sunshine vitamin, it does not mean that it is the only source. In fact that analogy is like saying that if a car can get you from Texas to California, then an air plane could not do so, because cars do it. Vitamin D can be sourced from any number of places, both beneficial and not so good. Not just the sun.
Kim Conneely says
The Vit D3 and Magnesium and Calcium issues you discuss are valid BUT only if you are not taking Vit. K2 with these three. The Vit. K2 completes the chain. Taking the other supplements without Vit. K2 is like making a cake without baking powder. It falls flat. Please read up on this and rethink your commentary.
Ann Johnstone says
So glad to hear you say that, Kim! Reports such as the above are so often inadequate at giving the whole picture: In this case, there is a need for a BALANCE of calcium, magnesium, Vit D3 and Vit K2.. It's so easy to 'throw out the baby with the bathwater', to use an old metaphor! All of the above vitamins/minerals are necessary in order for the body to absorb them them more effectively. I now take most of my calcium in dietary form, with just one easily absorbed calcium supplement, plus Vit Dr and Vit K2, in the mornings. In the evenings I take magnesium, as it assists with getting adequate sleep and has many other important benefits.
Several years ago I was hospitalized with severe atrial fibrillation. The cardiologist said he would 'stop-start' my heart the next day if it did not return to normal rate and rhythm. That crisis was averted through prayer. However I wondered whether my magnesium intake was adequate, and decided to take a more easily absorbed form of magnesium. (Never take magnesium oxide, as the body does not absorb it adequately).. Since then my heart has had a completely normal rate and rhythm. As a former medical science student and practitioner I like to research the most effective treatment for myself!
SunnySky says
Fantastic, Ann. Thank you for sharing.
More magnesium, please. 😉
Carrie C says
Another big thing is WHAT KIND of vitamin D are you taking? The big box stores, like the big W often sell D supplements that are petroleum distillates. Not good. When I was diagnosed with a vitamin D deficiency, I gathered up my organic sesame oil (protects the skin but does not block tanning rays) slathered it on and hit the sunshine. I felt better than I've felt in my life and lost 20 excess pounds without even trying! Again, as mentioned above, the right balance is of essence too. Don't just pop the D pill. K2 as well as other factors are involved. And, like with calcium which can be toxic if the wrong form is taken, do your research to find the right thing (ditto on magnesium) Always, it's better to NOT get your supplements in pill form, but for many, it's about the only way. People work, have long days in a building and drive home/to work/tend families...is that the best way? Probably not, but it is the way that IT IS. Supplementation is often necessary.
John S says
Lookup "Jim Stevenson Jr" Vitamin D Facebook page. Also lookup Jim's podcast interviews. He goes into all that. I will NEVER take Hormone D again, because first its not a vitamin.
Randi says
I was recently DX type 2 diabetic.. Eating lo carb high fat, was told d levels were low and to supplement 2000 iu with calcium. I realized that along with DX came some real healthy non processed food eating. Eggs every day, nuts, seeds. So I'm waiting to see my next levels before taking...
SunnySky says
Actually, we typically get plenty of calcium from our diet. What we really need is magnesium. Magnesium will naturally naturally raise D, if needed. Oh, and D3 uses up magnesium--not good. D3 puts calcium is soft tissue. 🙁
Check out this FB group, but be sure to read thethe group info: https://www.facebook.com/groups/1091015987575851/
Randi, more to consider:
http://www.calciumlie.com/type-2-diabetes/
God bless!
Vegangirl says
Dairy actually leaches calcium out of your bones, while the calcium in green, leafy vegetables provides a safe, healthy dose of equal or greater calcium. We need to stop promoting the myth that milk builds strong bones. Dairy is cruel, unsustainable and unhealthy. Go vegan.
Dan says
High five! Metabolic acidosis caused by excessive dairy intake is the leading cause of calcium deficiency.
Martin says
I was vegan for two years, and never got a single cold in all that time, but I noticed people in my vegan community getting cranky with the diet, and serious bone issues began to surface.
Raw A2 dairy is fine for bones, as long as it is unhomogenized, organic, from grass/hay-fed animals, especially goats, which is digested in 40 minutes rather than the 4 hours that it takes for cow milk to be digested, and is vastly less mucous-forming, so you don't end up having to try to clear your throat all the time with goat milk.
Animal B12, vital for human brain health, for instance, is destroyed by pasteurization. The figures for the incidence of osteoporosis are from people using large amounts of pasteurized, homogenized, mostly high A1 dairy, polluted with hormones, A1 milk being known to cause or exacerbate auto-immune disorders, like osteo and rheumatoid arthritis, and that is why they say to kids with asthma to drink goat milk instead.
The vegan diet is an artificially conceived diet, you cannot get real animal B12 in it, that the body can otherwise get from eggs, milk, cheese or meat, You can get Veg B12 from your vegan diet, from the plants, but that is a different molecule, and your brain needs animal B12, and the vitamin pills from the chemists are not what your brain needs either, as their molecular structure is different from real animal B12, which we cannot manufacture. If you risk malnourishing your brain with synthetic animal B12, the heavy price is possible dementia, and certain dementia starts to manifest after about 6 years without B12 supplementation of any sort when vegan diet is used.
Vedic diet, properly practised, as in India by some who maintain traditional culture, obtains milk from animals that are very often cared for like family pets, receiving protection from wild animals, bedding down in the safety of the family home grounds at night, and when they start to produce milk, as long as they are milked, they produce milk year after year without having to produce more offspring, unless more offspring are required. Society should not tolerate the intensive farms that we, unfortunately, do allow in the west, but they exist nonetheless, very, unfortunately. I get my goat milk from a non-intensive farm, where the goats are quite well-cared for. We don't have to tolerate intensive farming, and we don't have to stop using milk. Synthetic animal B12 vitamins that are not the same molecule could leave people mentally damaged in later years, and sadly, I keep meeting naive people who are bringing up little kids on vegan diets, albeit with the best of intentions, who have no knowledge at all of these issues, and though I manage to educate a few, there are vastly more who I never get to speak to who are sadly damaging their kids brains irreparably.
yasss says
the dairy industry is so cruel. all they provide for us is cruelty and ultra pasteurized dairy that offers little nutrition and benefit. i've been looking for raw milk in NYC but it isn't easy to find.
Suzanne says
You can find raw milk in New Paltz, not too far from NYC: http://www.oldfordfarm.com/raw-milk.html Their contact info is on their home page. You can also join a local chapter of WestonAPrice.org and find the milk that way.
elisabeth p mehl says
That is correct, Scandinavians, ( like me ) has the highest consumption of diary products in the world, but also the highest osteoporosis in the world. Diary is the least recommended way to get calcium, get a slowjuicer and a blender and start getting back your health! A plant based diet is proven always to be the most healthy way to live, you live longer and with less diseases. You can gooogle all you like and every actual study ( not just a text in the meat information page ) will tell you this 🙂
Ann Johnstone says
So glad to hear you say that, Kim! Reports such as the above are so often inadequate at giving the whole picture: In this case, there is a need for a BALANCE of calcium, magnesium, Vit D3 and Vit K2.. It's so easy to 'throw out the baby with the bathwater', to use an old metaphor! All of the above vitamins/minerals are necessary in order for the body to absorb them more effectively. I now take most of my calcium in dietary form, with just one easily absorbed calcium supplement, plus Vit D3 and Vit K2, in the mornings. In the evenings I take magnesium, as it assists with getting adequate sleep and has many other important benefits.
Several years ago I was hospitalized with severe atrial fibrillation. The cardiologist said he would 'stop-start' my heart the next day if it did not return to normal rate and rhythm. That crisis was averted through prayer. However I wondered whether my magnesium intake was adequate, and decided to take a more easily absorbed form of magnesium. (Never take magnesium oxide, as the body does not absorb it adequately).. Since then my heart has had a completely normal rate and rhythm. As a former medical science student and practitioner I like to research the most effective treatment for myself!
Barbara says
what is an "easily" absorbed calcium supplement
likewise...what is an "easily absorbed" magnesium supplement
Di says
As recommended by my nutritionist (who has a Master's Degree in nutrition), magnesium glycine and calcium from microcrystalline hydroxyapatite.
Carrie C says
Magnesium L Threonate
Barbara says
this is a question...not a comment. I have been making "green smoothies" for about a month (breakfast). They consist of either spinach or kale or a mix plus some fruit and protein powder. All organic. I have wondered what...if any...effect the use of the Vitamix on the greens has with regard to nutritional value or absorption. I am assuming the fiber content is negated....?
SunnySky says
Amen!
Great book on the subject:
http://www.calciumlie.com/get-calcium-dont-think/
Sean says
Why are vegans so stupid? If you're going to make claims at least try to explain the rationale. Dairy is rich in calcium, yet you claim it somehow lowers it. You then conclude your statements showing your real motivation; you believe the dairy industry is cruel, therefore you will believe any propaganda that tells you dairy is bad for you.
Your ancestors treasured dairy products. They would laugh at the notion of chewing cud when fresh healthy milk was available. Excessive greens are a great way to get kidney stones via the oxalates.
I have never met a healthy vegan. History shows the weakness of veganism; it spits in the face of our ancestors. Any weight they lose is usually just muscle. They have to take endless supplements (B12, zinc, taurine, selenium and often many others).
There might only be a temporary benefit from lack of meat to lower the protein levels of cysteine, tryptophan and methione. Eventually it will just cause one to be weaker, vs if the person ate meat.
There is nothing immoral about killing animals for food. Many small animals are killed to harvest vegetarian/vegan crops by the way. Endless rodents slaughtered through the harvest.
I often fantasize about sprinting about a deer and killing it with my bare hands and eating its liver fresh there and thanking the Creator for the blessing of the food. Eating meat gives strength, it is time you learned to embrace it. Away with your weakness. You sicken me.
Dc says
Ron Swanson!
Marie Page says
You know Vitamin D3 is not in foods in general so to get it from that source in adequate amounts is near impossible. A 10 minute tan, outside in summer and at a salon in winter can give you 10,000 to 20,000 units of Vitamin D3 through UV light reconstruction. It also uses cholesterol to process the Vitamin D3 and double benefit. If you go to GrassRoots Health you will see a chart that states Vitamin D3 kept at even levels over the full year can protect up to 77% against ALL cancers and some other serious diseases. Internal cancers are on the rise, the sun don't shine there!!! Dr. Marc Sorenson wrote the book D3 and Solar Power for Optimal Health. A very good read as it relates many chronic illnesses to the healing power of Vitamin D3. If we were meant to ingest it we would find it in lots of foods! It is really a hormone. It is also predicted there will be a $113 billion dollar medical expense down the road from our sunscare message. I highly recommend that you put the sunblock away as well ... check yours out on Environment Working Groups site ... they study them and for sure they are not safe!! Go organic if you do have to use one or cover up after an appropriate amount of sun. Everything in moderation people. When I asked for a Vitamin D3 lab test to see what my level was at because I tanned twice a week and would bump that up if it wasn't high enough, my Dr said "YOUR DON'T GET ANY VITAMIN D FROM TANNING BEDS". This type of ignorance is tragic in the medical profession because they learn what university want them to learn, sometimes you just have to look outside the box. Needless, it is hard to have respect for professional that are that closed minded no matter how book smart they might be. Vitamin D3 affects the immune system ... we need it, go get a little sunshine today, and be happy!!
sandi says
Here here!
Donna says
Yeah, well great. I adhered to the "go outside without sunscreen for 10 minutes a day for natural Vid. D." this past summer. Now I have ugly white splotches all over my legs from doing just that. 🙁 My Derm says it's genetic. But going out in the sun triggered it.
Sandi says
Shining on your face only is fine.
Katie says
I have been taking Carlson vitamin D3 for over a decade. My doctor recommended it as I had a lot of skin cancer from suntan abuse in my younger years. My calcium level is perfect..
I think the recommendations here are lopsided. Dr Holick. - Who has done extensive research and pioneered the need for vitamin D for health. recommends a minimum of 40 on your lab work for vitamin D – not 20. Protects against all auto immune disease is and cancers. Look at the big picture.
SunnySky says
I went to a dermatologist recently to make sure some spots on my face were ok; thankfully they are!
But, she gives me samples of moisturizer, one with color tint, and one without--but both have SPF. No way!
Dee says
If I had it to do over (I'm 60), I would religiously wear sunscreen on my face and reapply every 2 hours. I used to have perfect skin, now I have brown spots all over from sun damage and signs of collagen loss, with extensive lines and wrinkles around my eyes. Go without sunscreen on your arms and legs to get natural vitamin D, but protect the delicate skin on your face!
Steve says
Calcium and Magnesium are 2/4ths of the picture when it comes to D3, D3 obviously being 1/4th...what you haven't mentioned is K2!
I always recommend when people ask about D3 supplementation in regions with cold winters that Calcium, Magnesium and K2 are equally as important.
Connie Moorhead says
Yes, my Vitamin D levels have tested low. My doc put me on supplemental D - 10,000 IU D3 with K2. (pharmaceutical grade) some time ago. The last lab showed it had improved a lot, but it isn't in the proper range yet. He suggested I take it with my dinner containing fat so it would be absorbed better. My calcium level is too high, so he wants me to back that off some.
Jacqueline says
I had DVR in my left leg. As a result was taken off of K and green leafy vegetables due to its assist in the clotting factor. How does K2 differ from Vit K.
Does it affect blood cl9tting?
Jacqueline says
Correction DVT ***
Daze says
K2 does not cause clotting formation as k1 assists in:)
Lew says
Vitamin D FORTIFIED milk, also FORTIFIED with Vitamin A.
Catherine says
Hi Lew,
Whole milk naturally has vitamins A & D. Because they are fat soluble vitamins, they are found in the fat of the milk. When the fat is reduced, as in skim, low fat or 2% it is required to add synthetic vitamins A & D in.
“We are required by law to add vitamins to all of our fluid skim / fat free / nonfat milk, fluid lowfat (1%) milks, and fluid reduced-fat (2%) milks. These vitamins are fat soluble and a certain amount of them are lost when the fat levels in milk are reduced.” -Organic Valley
Thanks for reading!
Abundantly,
Catherine
Matt curtin says
Thanks katherine good to know!
Mary TItus says
Hi Ken, 600 IUs of vitamin D3 won't even scratch the surface to bring levels up substantially which is what you want to do. I take 10,000 IUS a day accompanied with magnesium, zinc and vitamins K1 and K2. Vitamin A should be added but I am not quite sure as to how much I should take.
Mary TItus says
The vitamin D that is in milk is not nearly high enough to scratch the surface of optimal vitamin D serum levels..
L says
Careful of the added Vitamin D in milk and other foods as it is generally Vitamin D2, which is synthetic and will cause insomnia. Should look for Vitamin D3, which is natural and absorbable to the body.
Benny says
Just like many others I have a low vitamine D level in winter times. I know this because last year I have tested my blood. Everything was fine except for the vitamine D and iron. I don't take supplements though, not for vitamine D that is. I also cramp up very easily so I have been told magnesium will help. So I have this supplements called ZMA, it's Zink, Magnesium and Vitamine B. I was told I would fall asleep more easily and sleep more deep. But when I started to take those pills I actually woke up 3x a night. So I don't take them anymore. I'm very skeptical nowadays about pretty much everything. The only thing I rely on is this small BIO shop in my hood. About the vitamine D. I'll just wait 'till summer gets back in town 🙂
Heather says
OK, so what about those of us who live in the far Northern hemisphere? I am told to take vitamin D supplements in the winter because we get 5-6 hours of sunlight a day at best. And that is when the sun is shining! Also, when it's -10 out, I'm not exposing my bare skin to the elements to catch some rays.
I feel you have not addressed this part of the vitamin D supplement necessity.
Kezia @ Super Naturally Healthy says
Great artical - I am currently just research best source of vit d and have been weary of supplement other than fermented cod liver butter oil. I do think some of our sun phobia and low cholesterol emphasis adds to the problem and nutrients are always best found in actual food - plus I will be trying out you egg shell recipe too I hate wasting all the shells we go through so hooray to find a healthy use for them 🙂
Van Wayne Dacayo says
Vitamin D3 & Calcium
Cynthia Padi says
I take vitamin D supplement. This is because my doctor means thatI need it. I have always had my doubts about how it works though. And talking about the sources . I really doubt if it is doing me any good. I do not drink milk because I feel really sick anytime I drink milk. But I try as much as possible to a well balanced diet. And I think I gain a lot og vitamins from my food since I rarely get sick.
Mo Hoyal says
My doctor said I am low in Vitamin D and to get on this. I don't drink milk any longer and do eat a balanced diet so what in heck am I supposed to do? I am out in the sun and healthy otherwise. One other thing.....I wonder if taking a statin is leaching some important vitamins from our systems? Don't like them but have to take for high cholosterol that is heredity in my family.
Mary Titus says
One thing, statins do deplete the body of vitamin D.. I am surprised that your doctor did not give you a good vitamin D supplement. Also, due to the fact that vitamin D needs cholesterol to be properly utilized by the body, it will naturally, cause a rise in cholesterol so please make sure that the doctor is aware of this and always request your cholesterol ratios AND triglycerides to get a more accurate reading on your cholesterol. It is the ratios between HDL/LDL /VLDL and triglycerides that count.
Di says
Read "The Great Cholesterol Myth " by Dr Stephen Sinatra .
edgar aquinde says
blood test result @ucsf--low vit d. was prescribed vit d2, 50,000 iu, every week for 1 month then every month until gone. given 9 total capsules. last test, vit d level went up by 10 but still not on minimum. doctor/nurse did not even discuss that it takes 3 pillars--calcium,magnesium,k2 for vit d to work well. ignorance or wasn't taught in med school? i prefer sunshine myself while exercising in moderation and eating vegetarian/vegan organic. wish conventional medicines would concentrate in prevention of diseases and surgical intervention, chemo,radiation,etc as last resort. this will improve the healthcare debacle and more people will be happier. pharma/medical institutions & other businesses will not make much money, but who cares. remember---DO NO HARM.
Di says
D3 is the right supplement , NOT D2, but most doctors don't have a clue about anything related to nutrition .
Dan says
Wow, Chris MasterJohn clearly doesn't have a bloody clue what he's talking about.
Westonprice foundation = bias pseudo-science wrapped in a grassroots "common-sense" wrapper. The meat and dairy industries "folksy" propaganda machine.
johny longshot says
Bah your telling people taking a vitamin D supplement is not as good as drinking poison milk ? Gimme a break and do some research on milk!
javier says
I don't understand if your against supplments why is
fermented cod liver oil ok?
Polyunsaturated oils are VERY unstable, oxidizing quickly when
exposed to oxygen, light and heat—even just sitting in a bottle, but
also when they go into our bodies—and turning rancid. (including
omegas) Also Fermented foods require a glucose source to create
(metabolize) a by-product e.g. lactic acid that prevents the food from
decomposing. The result is a pleasant sour taste that one would find
with sauerkraut, pickles, yogurt, etc. Cod liver oil has no glucose
and cod livers have very little glucose (mostly protein, fat, water
and some minerals). The livers and the oil simply go from fresh to
rancid in a short period of time. If left to continue decomposing the
oil will become putrid leaving a foul smell and taste.
Furthermore, Cod, like Shark, are long-lived fish. As they go about
living for years and years, and during that time, they accumulate
environmental toxins. And the toxins are most concentrated in the livers. So when you drink
Cod liver oil, you should expect environmental toxins! That just makes
sense!
Sadly, atlantic Cod is an over-fished and threatened species.
Why not just eat more fish and liver and gain similar yet better
benefits since it's a food source?
jules says
It depends. When you are sick (like really sick not just flu or any thing) it is not a bad idea to look at supplements. Of course you should look at the cause after that as well. But sometimes this cause is not just a cause but like a co-incedent, they happen at the same time. It is hard to find out what is first.
Vitamin D is also important for our nerves so if you are deficient you should look into it, especially when you don't live in Arizona or Spain. It's the sun that you need, or otherwise some vitamin D.
Mary Titus says
From my experience, vitamin D is a very important at optimal serum levels. I began experimenting with vitamin D with a forum group several years ago. We had decided to take considerably high doses just to see what would happen. Being pre-diabetic, I noticed and immediate reduction of blood glucose levels . Over time, however, I noticed an incredible and unexpected improvement in my allergy symptoms. I had had horrible allergies once I moved to CA 15 years ago. Because of the lack of real rain, pollen and dust hang heavily in our air. I would become congested. I sneezed heavily and my sinuses became blocked. The symptoms did not vanish but they improved beyond my wildest dreams. I concluded that it was the vitamin D that helped with my symptoms. Remember, I was not thinking about my allergies when I began experimenting with Vitamin D. When I began supplementing with vitamin D as I had mentioned earlier, I was taking high doses of this steroid and I have discovered that it is the high doses that offer real relief. I have also noticed that as my blood levels dissipate my allergies worsen.
I went to the Vitamin D council's website to see if this was at all possible . I discovered the strong possibility of vitamin D having therapeutic properties over allergies. That one experience alone has made me an advocate of vitamin D . My ex-husband began taking it and it is the only supplement he takes although I try to encourage him to take the co-factors as well ( vitamin A, K1/K2, magnesium, zinc ). Along with the co-factors, this "vitamin D' community deserves a lot of attention.
Mary Titus says
I did not finish my comment with my ex husband. Something that I found astonishing was he noticed that his mood had improved significantly when he takes it. I had not tell him what to expect with vitamin D, nor did he research it. So for the past 4 years, he has been taking it o a regular basis.
Lynn Marie says
I agree with Mary. I test low simply because of age and I stay out of the sun. Right now I take prescription Vit D once a week. Let's not discount the recent studies that show the link between D and Alzheimer's. Vit D has shown to help clear the plaque that contributes to Alzheimer's.
Mary TItus says
One reason that vitamin D is discredited is it requires other nutrients to work properly such as magnesium and zinc. It also requires the consumption of fat and cholesterol to be properly absorbed. But when it is partnered with the proper minerals and other nutrients, as it should, it does become a vital nutrient for optimal health.
ken says
So you have missed another reason for low vita
Hyperparathyroidisum which I have been suffering from for over 14 years.
The parathyroid are 4 small glands in the next andre round the thyroid which act like small sensors, screening the blood for levels of calcium.
when it drops they produce a hormone which causes you to leach some calcium from your bones.
They usually remain asleep if you will until levels drop.
One or more of mine are constantly awake producing parathormone which raises my blood calcium.
When I was initially diagnosed through a random blood test my vit D levels were 32 nmol (uk)
They started to supplement me with a 600iu dose per day of vitD3.
After 18 months hey retested me and I had dropped even lower to 17 nmol which is pretty bad.
My symptoms were much worse.
I did some reading mainly from Charles poliquin and others who had mentioned large doses and started to up my intake.
I now take 2 doses of 35'000 in a week, 1 on a Tuesday and the other on and Friday.
My vit D3 levels are now always in the 120 nmol region and my symptoms have dramatically improved.
I would do some more reading before deciding on it and if your feeling tired, irritable, dry mouth itchy eyes, muscle and joint pain go get a blood test and check, it gets missed alot.
Anna says
Ken, I have the same problem with hyperparathyroidism and according to dr. Norman it is not a good idea to supplement D3 in our cases. Have a look at his website parathyroid.com He says it is protective that the body lowers D3 levels if your parathyroids are overactive!
John V. says
I disagree.... I have issues with numbness from Fibromyalgia andi seems taking D3 reduces my numbness the same day I take it.... Its link to warding off Multiple Schlerosis is very well documented. So i think you don't know what the heck you are talking about. Simply the most important supplement one can take. Nothing comes close. Not even Vitamin C.,
Mary Titus says
John V...I agree
Mary Titus says
One thing for certain is proper nutrition is necessary for good health. This requires all minerals , vitamins and natural steroids ( vitamin D ) to work with each other. If you are missing one nutrient, you will become deficient in at least one other nutrient. There is no such thing as once being better than the other because they rely on each other.. That is why the vitamin D council refers to magnesium, zinc, vitamins K1 and K2 etc. as co-factors of vitamin D. Without them vitamin D is less effective and can even become harmful without it's "team " players. Plus they have additional jobs that go beyond the vitamin D team.. We must remember that
Sandy Vichery says
Although not everyone is deficient in Vitamin D, I myself have Hashimoto's Disease and a gene defect which does not allow me to store Vitamin D. I was in so much pain prior to supplementing I could not believe how much better I feel getting my level from 20 to 80 which is what my Integrative MD suggested. I take sublingual Vit D with K2 5000 iu daily (Amazon) as and it works great and I feel great so I agree not everyone may need it but I sure do!
John says
I too am skeptical of cure-alls and quick fixes. But I'm not so sure that dairy is a good source of calcium.
Harlan says
While I appreciate the information and research that has come out of the Weston Price Foundation I think your contrarian argument against vitamin D supplementation is flawed. Too many people in our society are just not getting sufficient sun exposure and vitamin D supplementation is a stop gap measure that benefits many.
sharon says
Hi all--
There's a reason why they called Vitamin A, Vitamin A.
I had read an article in the WAPF, or maybe it was the Price/Pottenger bulletin, that spoke of the dangers of any kind of large supplementation of any vitamin, fat--or water-soluable-- without sufficient Vitamin A to drive it. I agree with the literature I've read, that Vitamin A being master over the other supplements is key to best results.
Curious to hear from those trained more deeply/formally than I am. I'm able to testify I was my healthiest and lost weight easily when I was drinking raw dairy and taking cod liver oil, both daily. (Then I met my hub and all healthy eating was off the table for a while...)
Renee says
Sometimes we have to rely nohow we feel...I have had thyroid cancer, and supplement with bioidentical thyroid, Vit D liquid, as I can not be in the sun at all, and do take lots of magnesium and K2...and I feel so much better than I have in 30 years. Fear based information is dangerous for so many people...we are not robots; we all have different needs and need to respect what our bodies tell us.
Robyn says
Wow, thanks to all those who commented, especially those who have obviously done lots of research. I need to read all the comments again to take it all in.
Erika says
People quit going into the sun for fear of skin cancer which explains why there is this trend in vitamin D deficiency. One primary factors in this equation and the fear of skin cancer problem is excessive exogenic sugar intake in the diet and the weakening of immune function when exposed to the spectrum of cosmic rays i.e. UV radiation etc.
It really is a vicious cycle nobody wants to understand unfortunately because we are conditioned from birth to think that introducing excessive exogenic sugar especially high fructose corn syrup etc. to the diet and human body "is ok" according to who? Any official source I have seen contradicts hard cross validated empirical research (sugar industry has friends in high places?) when it comes to recommending a daily allowance (e.g. bleached flour causing diabetes in labratory rats?) and the introduction of excessive exogenic sugars and carbohydrates to endogenic human chemistry.
Myth: The brain and body need glucose and carbs to live or survive? (that is a false assumption)
Richard Lohaus says
I am getting my Vitamin D from liquid fish oil, D pills (lanolin derived) and fish such as sardines. Recently I cut back fish intake due to concerns about mercury. Catherine, would you be willing to address mercury consumption, testing, and/or detox in a future blog? Thank you for sharing this information on D, Richard.
Sarah says
So...what do you do instead?
Scarlett says
Hi I’m new to your site. I was diagnosed with osteomalacia years ago then years later with Lupus and RA. I definitely began feeling better after finding out I had low vitamin D levels then taking more. Lately I’ve been considering trying the new vitamin called Ritual. Any thoughts on this particular vitamin?
Janet Squire says
I stopped supplementing with Vitamin D a couple years ago after reading a very good article by Shane Ellison on it. I get plenty of sunshine all year long in Colorado and would rather get my D the natural way. Thanks for the informative post, most people are just blind sheep and will do whatever their robotic doctors feed them, even when it's wrong and dangerous.
Jonathan Frewing says
Indeed,. Vitamin D is actually a hormone. This means it has a band of efficacy. To understand this to the fullest, please study the work of neurologist Dr Stasha Gominak.
She has established, through a decade of sleep studies and EEGs, exactly what that optimal hormone level is, and can demonstrate it through REM sleep. This level of sleep is when all bodily repairs take place, so it is crucial to all health.
So now we have real data on which to base our vitamin D assumptions.
The vitamin D to gut relationship is also interesting, in that many gut flora feed on vitamin D. When D drops, the gut flora die back and it transpires that these flora are the ones that make supplemental B vitamins.
As soon as the vitamin D level begins to normalise, the body's demand on B vitamins increases, as it needs these for repairs. It is therefore advisable to supplement with B vitamins while normalising D. Then, when the gut flora are back on their feet, it is important to stop, or dramatically reduce the Bs.
I encourage you to scrutinise Dr Gominak's work. It appears to be the only scientifically validated approach to this thorny question to date.
Catherine says
Thanks Jonathan, I will definitely be looking into her research!
Abundantly,
Catherine
Richard says
The benefits of having Vitamin D levels around fifty where your receptors are saturated is well documented. I refer all my patients to vitamindcouncil.org. It should clearly be paired with vitamin k2. Your point is well made that natural sources for all these nutrients are most likely the best sources. Secondly, having better D levels affects other numbers, as you point out. As a physician who has to deal with internet misinformation, I would like to point out, that you have a very powerful role with your readers. This article is confusing because the benefits for the immune system with good vitamin d levels is profound. Tremendous effects on cancer metastasis ( nagalase ) , flu prevention, and allergies, Effects in CVD, MS and other immune mediated disorders. I wish your article was titled, how to maximize supplementation of vitamin d. There are numerous great points that you make. Otherwise keep up the nice work. 😀
Catherine says
Thanks Richard for your thoughts and for joining the conversation!
Abundantly,
Catherine
Jacqueline says
Can’t take vitamin d3 my level is 9 what to do?
Selia Fernandes says
I have hypothyroid and am low in vitamin d , also borderline o n ca)cium. Whenever i take d 60K do ypu recommend taking in calcium too.
Know Supplements says
I love to read and write about supplements and vitamins regularly, but I never thought of that Vitamin D do have side effects. Means it comes from a natural source. But somewhere this information shocked me too and I am happy to that I find this page. Good Job Catherine...
Olga says
you can ask your doctor to place you on other type of blood thinner (other than warfarin/coumadin) so the food will not interact with the medication