 Did your grandparents have thyroid problems such as hypothyroidism? Mine sure didn't, which is a stark comparison to the millions of Americans suffering from thyroid problems today. So why didn't your grandparents have as many thyroid issues [specifically hypothyroidism] as we do today?
Did your grandparents have thyroid problems such as hypothyroidism? Mine sure didn't, which is a stark comparison to the millions of Americans suffering from thyroid problems today. So why didn't your grandparents have as many thyroid issues [specifically hypothyroidism] as we do today?
In my opinion, it's really quite obvious...
1. They ate and used the 'whole animal'
Your body (especially your liver) needs the amino acid balance that is achieved when you eat the "whole animal." If your liver is malnourished by not eating enough of the right kind of proteins, it can have a detrimental effect on thyroid hormone conversion.
2. They got more Thiamine (B1) in their diet
Thiamine deficiency is alive in well causing symptoms such as digestive issues, irritability, low blood pressure, depression, fatigue, and issues digesting carbohydrates.
You see, thiamine is needed to create energy your body and is used up when you process carbohydrates. But, today in our processed-food laden land, the thiamine typically found carbohydrates is stripped out during processing or empty carbohydrate foods didn't have any thiamine to begin with. This creates the perfect storm for thiamine deficiency, as your body quickly uses it up faster than you are taking it in.
Initially, this is why the grains were enriched with b-vitamins, including thiamine decades ago. But the water soluble form used for enrichment doesn't have the best bioavailability and then there's the popularity of grain free diets.
The bottom line here is that thiamine deficiency is common and research shows it can help with thyroid-related fatigue. [10]
You can read more about thiamine deficiency here.
3. They didn't intentionally eat less and exercise like crazy
When you have a chronic energy deficit (fewer calories coming in than going out), over time your body starts to think food is scarce. To make an analogy, think of your body like a house. If you're not making enough money to pay your bills, what do you do? You turn down the heat in your house to compensate, turn off the lights when you're not in the room, and perhaps even fire your cleaning lady.
Your body operates in a similar way. When there are not enough calories coming in, your body saves energy by reducing body temperature (slowing the metabolism), turning down digestive juices (making digestion weaker), reducing the pulse, and slowing thyroid function (resulting in less energy and T3). This is a built-in survival response by the body, to help you go longer on less food as your body chooses short-term survival over long-term health. This is often induced through over-exercising and dieting.
Listen to my full interview on this topic here for more.
4. They didn't subsist on nuts, quinoa, GMO soy, and kale
When you ate dinner at your grandparents' house, did your meal consist of nuts, quinoa, GMO soy, and kale? I didn't think so. Harder to digest foods like these often both poorly digested and irritate the gut; resulting in an increase of endotoxin (lipopolysaccharide or LPS) that suppresses thyroid function.
"Dysbosis and poor digestion prevent the body from successfully eliminating unnecessary estrogen, and toxic levels of this powerful hormone build………. Excess estrogen binds the thyroid transport proteins so that thyroid hormones cannot get to the cells to do their jobs, causing hypothyroid symptoms." -Dr. Kharrazian
Get the un-digestable foods out of your diet, and instead focus on easy to digest foods to support thyroid function.
5. They didn't self-induce hypothyroidism with bodily stress from dieting (particularly low-calorie and low carbohydrate diets)
Both low carbohydrate and low-calorie diets are still king in the dieting world, due to their ability to provide fairly quick, but short-term weight loss (read: endless yo-yo dieting). Unfortunately, they also slow the metabolism, directly impacting T3 (active thyroid hormone) levels, which can result in self-induced hypothyroidism. According The Journal of Clinical Endocrinology and Metabolism, dietary carbohydrates are an important regulatory factor in T3 production.
Dr. Ray Peat, PhD, agrees: "The liver provides about 70% of our active thyroid hormone, by converting thyroxine to T3, but it can provide this active hormone only when it has adequate glucose."
Nutrient-rich sources of sugar (read: carbohydrates) should be a mainstay in your diet. If the word "sugar" is scary to you or you've blacklisted it from your diet, you might want read this for some context.
6. They didn't have as much exposure to fluoride from their water supply
Fluoride was widely used in the water supply by 1960 when fluorinated water reached approximately 50 million Americans to help prevent dental caries. Recent studies however, show fluorinated water can double the risk of hypothyroidism! This risk makes it a great time to invest in a good water filtration system (like this). Read more about all the reasons you want to reduce your exposure to fluoride here.
7. They weren't overly reliant on "medicine" to fix things that should be fixed with common sense
Imagine for a minute you are Jane Doe. You feel tired, fatigued, and have no energy-all the time. You go to your doctor and he discovers that you have low thyroid function, and he puts you on Cytomel (T3) or some combination of T4 and T3. Initially you feel better, because T3 is the body's form of energy - so in a sense you are taking an "easy button" to get more energy. With this increase in energy, you start working out, doing more around the house, and all those things you were unable to do previously. You feel a lot better at first, but then you start feeling worse... Because you didn't change your diet and lifestyle habits and you did not back up that energy production with a nutrient dense diet. You then make the decision to go back to your doctor and he ups your dose…
What is the problem here? If you take thyroid medication without addressing the root cause behind it, which is most often a nutrient and cellular energy deficiency, then you are essentially purchasing that "increased energy" with a credit card! If your body doesn't have the nutritional stores to pay for that energy, that thyroid medication could be digging you into deeper and deeper nutritional debt.
8. They didn't overload on calcium or vitamin D3
The average American today gets far too much calcium relative to potassium. Typically, one isn't taking in too much calcium from food sources per say (although one could over-do it), but instead from calcium supplements, calcium fortified food, and/or they have increased calcium absorption from taking high dose vitamin D3. Part of vitamin D's job is to tell your body to absorb more calcium from your food, pushing calcium levels even higher in the body, and pushing potassium levels lower.
Pair that with a chronically low intake of potassium from fruits and vegetables, and you have yourself some powerful nutritional forces messing with your thyroid hormones ability to do its job. This often manifests with symptoms like fatigue, brain fog, low body temperature, blood sugar issues (hypoglycemia), and sluggish digestion.
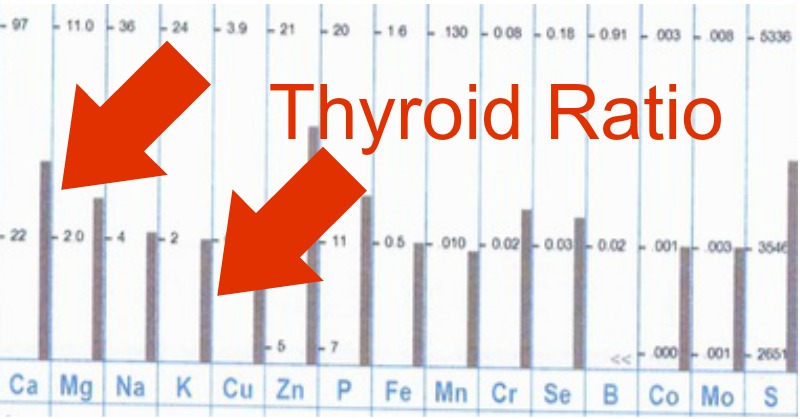
In hair analysis we look at the calcium-to-potassium ratio to assess how well your thyroid hormone function is supported from a mineral perspective. If you have a high ratio it represents lower function, expressing as low thyroid symptoms, or making existing symptoms worse. If your potassium levels are lower (often due to low carb dieting, dieting in general, or stress) this would deepen the impact.
Here's a little example of what I'm taking about. Below you'll see we're looking at the calcium (Ca) and potassium (K) levels to assess thyroid health from the hair tissue mineral perspective:
If you're curious if your vitamin D supplementation has your thyroid function in hot water, you'll want to read this and consider getting a hair analysis, to see how your calcium and potassium levels are affected.
9. They didn't overdose on vitamin A
I know what some of you are thinking, "but vitamin A is important for hormonal balance, thyroid health, and fertility." But let me show you how easy it can be to get too much, especially considering once "seasonal foods" high vitamin A foods are often now available on demand year-round. Here's an example of some commonly eaten "health foods" that are high in vitamin A:
- Liver 338% DV in 100grams
- Sweet potatoes 769% DV in 1 cup
- Carrot 44% DV in 1 medium
- Kale 206% DV in 1 cup, chopped
- Salmon 25% DV in 100grams
- Butter 11% DV in 1 tablespoon
- Cheddar Cheese 12% in 2 ounces
- Eggs 24% DV in 3 hard-boiled eggs
Do you see how one could easily get the daily value of vitamin A through eggs, a few tablespoons of butter, and a carrot or two? Then layer on a multivitamin and possibly other supplementation containing vitamin A that doubles or triples what they are already getting from food? Then they also might have a history of using the birth control pill (which increases vitamin A), use of vitamin A containing prescription drugs (think acne drugs in particular), sunscreens with added vitamin A and beauty creams that puts their intake way over the top. You'll definitely want to read all about the signs of vitamin A toxicity here.
It's not a life sentence, it's your habits
Thyroid problems (specifically hypothyroidism) are often a consequence of your diet and lifestyle. Adopt a nutrition plan that gives you enough food and calories to support your body's cellular metabolism and energy production before jumping on the prescription solution bandwagon for your hypothyroidism.
P.S. If you want more practical tips (just like these), you'll want to enroll in the Thyroid Reset Bootcamp. Read more about it here so support your thyroid health with food!
What do you think - did your hypothyroidism occur after heavy bodily stress like childbirth, excessive exercise, or weight loss efforts? Please share in the comments!
PIN IT:
References:
- Loucks, Anne B., and Edward M. Heath. "Induction of low-T~ 3 syndrome in exercising women occurs at a threshold of energy availability." American Journal of Physiology 266 (1994): R817-R817.
- Peat, Raymond, PhD. Unsaturated Vegetable Oils: Toxic. Retrieved from http://www.raypeat.com/articles/articles/unsaturated-oils.shtml
- Spaulding, Stephen W., et al. "Effect of caloric restriction and dietary composition on serum T3 and reverse T3 in man." The Journal of Clinical Endocrinology & Metabolism 42.1 (1976): 197-200.
- Spaulding SW, Chopra IJ, Sherwin RS, Lyall SS. "Effect of caloric restriction and dietary composition of serum T3 and reverse T3 in man." J Clin Endocrinol Metab. 1976 Jan;42(1):197-200.
- S Peckham, D Lowery, and S Spencer. Are fluoride levels in drinking water associated with hypothyroidism prevalence in England? A large observational study of GP practice data and fluoride levels in drinking water. J Epidemiol Community Health doi:10.1136/jech-2014-204971
- Prof. Dr. Andro. Thyroid Issues? Low Energy Intake Triggers Low T3 / High rT3 Syndrome in Exercising Women >19kcal/kg LBM Avail. Energy Required. Low Carbing Worsens the Impact of ED. Retrieved from http://suppversity.blogspot.com/2014/10/thyroid-issues-low-energy-intake.html
- Wikipedia.com. History of water fluoridation. Retrieved from https://en.wikipedia.org/wiki/History_of_water_fluoridation
- https://ggenereux.blog/
- https://pubmed.ncbi.nlm.nih.gov/24351023/
- Photo Credit: By Bryson Jack, Ministry of Information Photo Division Photographer [Public domain], via Wikimedia Commons
- https://www.mdpi.com/2072-6643/8/3/128/htm
- https://www.tandfonline.com/doi/full/10.1080/00325481.2019.1607414
- Photo Credit: Depositphotos.com/LiliGraphie




Kate says
Excellent article, but how does someone know if they are eating enough? For example, I am 175 lbs and I eat maybe 1400-1700 calories a day, while my Sister who is 120 lbs eats closer to 2000 calories per day. We are both sedentary (<5,000 steps a day...I can barely go up a flight of stairs now due to adrenal and thyroid issues). I understand that eating too little down regulates metabolism, but how do you know how much you are supposed to eat?
Jp says
How much you eat depends on you. Unfortunately there is no fast and easy answer, especially if you can't find a reliable MD or ND who understands thyroid issues. Look into Dr. Isabella Wentz, Dr. Mercola, Sean Croxton, Dr. Amen....if you haven't already...use them as a means to find more info. print it off and take it to your doctor. we are customers not patients. Best wishes!.
Lucinda Gonzalez says
I don't have ANY of these habits and I have Hypothyroidism when I can't find anyone else in my family that does or did have it. So how do you explain that?
lady tate says
Perhaps stress or environment causes? Many have thyroid induced anemia and do not know it because iron levels read normal often, and nutrition is good. Read comment below for more. Good Day! : D
Danielle Byrnes says
Completely agree with this article! I had meningitis several years ago, toxic breast implants removed and my body is still fighting to get rid of toxins today. It is such a journey but in it for the long haul! There is no easy fix that is the healthy or the right way! Thank you for the good read!!!
Jessica M says
Did you spend a lot of time swimming? A friend of mine got the same disorder and she swam in chlorinated pools. Research Hashimotos thyroid disease. Hope this helps.
Anita Clark says
They may have it, and it depend on the reference range at any particular time. 2011 ft4 12 to 22, 2015 ft9 to 19, 2023 ft 11.1 to 20, don't know the tsh range. These can also change within the years. Your family could only show borderline but still have it. That can include both or one side of our maternal and paternal families. These ranges can also be different in other countries. Also what a doctor told me is healthy thyroid is between both numbers of the ft range. As you can see from the ranges above these can give off false abnormal results.
Theresa says
Get your body fat tested and that should tell you your bmr, which will tell you your absolute minimum calories just to lay in bed all day. If you can't get that done, there are calculators online that can estimate it without the bf%, but with it will get you the most accurate
shano says
she could have parasites. and those can give you diabetes, particularly the common sheep fluke, in the pancreas or liver.
Everyone should do a parasite cleanse each year, or even quarterly. Dr. Clark has the best method, imho.
Jen says
I developed my thyroid issues during pregnancy and after birth it got much worse. I enjoyed this article very much. Lots of info and makes total sence. I have been on synthroid for 19 yrs now and some days I feel the same way I did before they eradicate my thyroid and put me on meds. Thanks for the great info. Can't wait to read more
Hazel says
To all the people asking what they should eat now, how much, and how many steps they should be getting...
I don't think you really understood the point of the article... it's not to obsess even more over things that you shouldn't be obsessing over in the first place. That obsession is driving you to behavior that has long-term negative health consequences, and you need to stop. Listen to your body, and just live naturally and normally. No obsessiveness, food pickiness, calorie counting, or fitbits needed. If you want the good health your grandparents enjoyed, it starts between your ears.
1) Listen to your body and trust what it's telling you.
2) When you're hungry, eat. When you're not hungry anymore, stop eating.
3) When you're eating, your body knows what it needs, so eat the things your body wants. Note: not the things you think you "should" want, according to some diet fad, or your friend Shirley, or what you read in a magazine somewhere, or some random study you read about (funded by god knows who... gee, wonder if THAT had any influence on how the results were analyzed? It's amazing how gullible some people are.) but what you actually want.
4) Understand that food is not a way to seem "better" than other people, or something to obsess over. It's food. It exists to fuel the body and to taste good, period, and has no more significance than that.
5) When you feel like walking or exercising, do so. When you don't, then don't. See #1.
6) If you're taking a double handful of vitamin supplements every day, STOP. Unless your doctor has advised otherwise, just one daily multivitamin in the morning is really all you should be taking regularly. Remember, you can OVERDOSE on vitamins and minerals, too. They are PILLS, not tic-tacs, and should be treated accordingly.
If all of this is too difficult after god only knows how many years of treating food as ego validation rather than fuel, obsessing over yourself, and so on... think of the most down to earth, unpretentious man that you know. The kind of guy whose idea of a good meal is a steak and a baked potato, and wouldn't even know what edamame is. Eat exactly like he eats (but in about 2/3rds the quantity he eats per meal) for about a month, and take a single multivitamin every morning.
At the end of that month, you'll feel like you're in your 20's again. I'm not kidding. How fast you heal from minor injuries will double. You won't be tired all the time anymore, and will have vastly increased physical stamina. You will likely notice a small increase in physical strength, as well. Your mind will be clearer, with very little if any "fog". Emotionally speaking, you won't experience even a fourth of the issues with anxiety/depression that you currently have.
If you weren't the sort of woman who is prone to VASTLY overvalue everyone else's personal judgments of you and your lifestyle, you likely wouldn't be in this position to start with, So, this might motivate you to make the change, as well -- When you feel so much better (and thus aren't whining, complaining, being lazy, obsessing over yourself, and having random outbursts) other people will respect you a lot more, too.
Try it, seriously. What do you have to lose, except unhealthy self-obsession, the resentment of those around you, and a reputation for being neurotic?
Walter says
Nice summation...
I couldn't agree more @Hazel. We have become lost in the analysis of what we take in and what we put out. We got lost in keeping up with the Jones and average Joe is no longer trying to be average (not that there's anything wrong with rising to your potential).
@Catherine... great article. I appreciate you taking us back to simplifying the whole "exciting" diet rollercoaster back to basics!!!
Lisa says
Wow! You made some great points, but in such a terribly condescending way. So unnecessary.
Mary says
I totally, totally agree. I got my hypo thyroid after alot of stress (difficult marriage then divorce, working ridiculously long hours and being anxious alot.) I have been cooking more nutritious meals and still working on my sleeping pattern. We have more stress than our grandparents because of family breakdowns etc. So when we learn to handle stress better, eat more natural foods and have better relationships, then things naturally improve. I am a testament to that and a better person for all the lessons I've learnt.
Jen says
You’re absolutely on to something. I thought of my father in law, who is a rural Indiana farm boy, 72 Years old who is healthy, wise and eats what he enjoys. I can name countless “let go and eat” people who are not irresponsible or unhealthy, but much better off. I appreciate your candor. You nailed this one!!!
Ravi kumar says
Control and Life Rule matter a lot. If these two things we can manage, no disease can control you. You can control this.
Thanks for the great article.
Michele Clow says
That was very interesting. My hypothyroidism came on after having three children and lots of diet and exercising afterwards. I felt like I was in better shape after having my kids than before. And then about the time my youngest was three, I started getting tired and unmotivated. I ended up gaining 50 pounds, sleeping all day and feeling very depressed. After I started thyroid medicine, I definitely felt better, but I am still struggling with my weight and energy level. I am trying to be on the Wheat Belly diet in a house where no one else is.
lady tate says
My circumstance similar. No wheat helped initially but then I ate pizza as a guest: darn! Then my levothyroxine began to lose its power for me and then became too much for my system, even in baby dosages. Read about a doctor researching on the problem: looks as though the thyroid (and body overall) suffer inflammation which causes a certain hormonal change suppressing the body's ability to process iron, despite adequate intake and readings. Ergo: anemia. I just began iron supplementation today. People have report good success w/ various regimens and nutrition. Keep looking ahead... it improves. Sometimes it can be awful, though... visit a doctor to be sure of things, and be careful! Many may not be aware of the iron deficiency component.... as it is relatively new. And study is ongoing. The afore mentioned researcher is Dr. Lisa Tussing-Humphreys Phd. at the U of Illinois Chicago. The hormone in question is called 'hepcidin'. Worth seeking such info out! I am taking chelated Iron 27mg 'gentle ferrous bisclycinate' purchased on Amazon. To cap my statement here, it seems that anemia and inflammation could be the major issues to address at the moment.... let's hope we all get well PDQ! God Bless!
Rebekah says
I have a similar story. Although mine was after having 4 kids. my youngest is 3 and I can't seem to lose the last 10-15 lbs. I did a few triathlons and weight training since she was born and last year I had no energy and gained more weight. Did low carb and I felt good for awhile and then no energy again and couldn't lose weight. I've decided to forget it and just eat lots of real food. I hope it will make me lose weight but if not, then at least I have energy to do stuff with my kids.
Eleni says
Look into aip diet
Paul @ Eco Stores Direct says
It's unfair to say that it's a new 'thing', but it does seem to have increased. Really interesting article
Stacy Hancock says
I'm pretty certain my mother's mother had an undiagnosed thyroid issue. I don't necessarily thing they didn't have issues with it back then, I just don't think it was well diagnosed. I don't think a lot of things were understood back then or treated safely. My grandmother was subjected to shock therapy, for example. And childbirth. Twilight sleep, anyone? I absolutely agree with several of the points having a lot to do with the difference in their health and ours today, but I think it's a stretch to go so far as to suggest they didn't have thyroid issues because of the above..
Side note- heavy metal toxicity post WWII would be a better suggestion to explain the potential increase in thyroid issues, in my opinion. Heavy metal toxicity absolutely affects the thyroid function.
Ren says
Stacy,
I agree that thyroid problems existed back then but also for many of the same reasons as today. My grandmother had a thyroid problem, but she also had severe mental issues. You mention that one grandmother had ECT ~ that is not uncommon today and can be a very effective treatment for people with mental illnesses. Many people with mental illness have thyroid issues. Another problem is medications. Lithium, which has been used in medicine since the 1800s but came into higher use around 1948 for treating mental illness (especially bipolar) is extremely hard on the liver and can cause clinical hypothyroidism (though it can be reversed) if use is discontinued. However some research exists that supports higher levels of T4 to combat mental illness. Also, some of us have been checked for heavy metal toxicity and don't have any problems. Now that we don't use lead based paints, much of that is non-existent unless you live in developing countries or extremely poor areas.
This article has some good points because, yes, we do eat very differently than our grandparents but then foods are chemically modified and animals are injected with hormones that are relatively new to mainstream diets. Another reason why people need to be aware of what they eat and where food comes from. Growing up we didn't have all of the low-fat and no-fat options on foods that have flooded markets today and are horrible for your body. On top of that, most people eat an incredible amount of white, processed sugar and flour that our grandparents didn't consume. The body will attempt to adapt to changes in eating habits, thus we now have many gene mutations that didn't exist and yes, today's medicine can now detect these things through advanced medicine and the complete mapping of our genome.
In general, we have been led astray on what a healthy diet consists of, at least in America. If you travel to European countries, they have healthier diets with less issues, but they still eat the way our grandparents did so draw your own conclusions. They also don't allow thousands of ingredients in food and personal care products that America allows and American companies alter their items to fit European guidelines but continue to poison our products.
As a side note ~ everyone who thinks they have gained an exorbitant amount of weight by having hypothyroidism, check again. The average person only gains around 10 lbs in direct relation to hypothyroidism; the rest of the weight is caused by poor eating habits and a sedentary lifestyle due to lack of energy or mental illness or laziness. I have hypothyroidism (caused by Lithium) and have been able to lose weight through a healthy lifestyle and maintain a healthy weight that is not overweight. I have also had periods in the last 20 years that I didn't need to take medication for hypothyroidism and was perfectly fine (a 6 year stretch was the longest period).
It's important to take your health into your own hands. Know what doctors are doing and ask questions.
lady tate says
Guess you haven't yet heard about some of the ongoing research involving thyroid induced anemia? See above comment!
YVONNE says
My grandmothers younger brother died from thyroid disease when he was 2 years old.
Stacy says
Mine came from chemotherapy, unfortunately, but you have some great information here ~ at least based on what i have learned, so far...
Angie says
Mine is from chemo drugs I am taking and will need for the rest of my life.
loa says
I agree with some of those but not the diet part. My grandparents ate a nearly exclusivEly vegan diet, even when "vegan" was a virtually unknown word (i remember eating lots of tofu, fruit, and fresh bread when I visited them). My mother's brother grew up and married a woman who prepared animal based food every day. He ended up getting a triple bypass before the age of 50. Meanwhile my grandparents went on to live quality lives and both lived to be nearly 100. I know way to many people who eat real butter, meat, eggs who are sick fat and living on drugs. I''ll stick to my whole foods, vegan diet and will continue to enjoy perfect health for years top come.
Isabel says
This is such a interesting but also very confusing topic, Ioa. I've seen people thrive on Vegan diets but others who have developed terrible problems with the same diet. The same goes for Paleo type diets. I wish it was as simple as one diet working for all. You're lucky that you are so certain. I live with suspicious about all extreme diets including these Paleo-meat-eating diets as well as Vegan diets. I wish it was simpler
Dee says
"My mother’s brother grew up and married a woman who prepared animal based food every day. He ended up getting a triple bypass before the age of 50. Meanwhile my grandparents went on to live quality lives and both lived to be nearly 100. I know way to many people who eat real butter, meat, eggs who are sick fat and living on drugs. I”ll stick to my whole foods, vegan diet and will continue to enjoy perfect health for years top come."
My parents' diet consists of red meat, pork, chicken, real butter, eggs, sugar, white flour. They love bread and baking cookies. I followed a Vegan diet. I now have a goiter/hypothyroidism. My folks never had a thyroid issue, Mom is 87, dad is 94. They are still active, neither is overweight.
Go figure.
It's not one diet works great for everyone.
Sonya says
My great grandmother was born in 1898 and lived until she was 102. She was still active and gardening in her late 90s, growing vegetables, living a healthy active life. But she had a goiter on her thyroid the size of a lemon for many many years.
Her daughter had a low thyroid and was on medication for as long as I remember. Now my sisters and I have thyroid issues too, and I suspect my mum does as well. So I wouldn't be surprised at all if it's hereditary
Anne says
The lack of iodine in today's foods is the primary cause of hypothyroidism.
Ren says
Most people (in the USA and developed countries) eat iodized salt (and too much of it quite often) and foods with iodine (some seafood, dairy, cranberries and some organic beans and fruit). Iodine deficiency is the largest Worldwide cause, but isn't really a factor unless you're in a developing country.
Vesna says
Hi, this comes maybe a little too late in this thread, but just wanted to say that iodine deficiency was definitely the main factor for my hypothyroidism, and I do live in a so-called 'developed' country. It took only ten days of increased iodine intake for me to have my thyroid values in perfect range again. Unfortunately, what you're saying is not true - most of the food does not contain enough iodine, as most of the soil is also iodine-depleted.
Nicole says
No premade foods contain iodized salt. Because companies aren't required to use it, they don't. Unless you cook every single meal at home, you're probably deficient...
Josephine/Pinky says
My mother, who is now 88, has had thyroid problems all her adult life, before and after having kids. I can't remember her not being on thyroid meds. My doctor checked my thyroid and said it was fine. I think there are a lot of factors that have influence on this. The best thing is to research your symptoms, and talk to your doctor. Run some blood tests, and do what you feel is best for you.
Tracy says
My Grave's Disease (hyperthyroid) started after an 80 pound weight loss over a year, some by eating a nutrient-sense, whole food (including organic meat) diet and exercising. I never felt better at 50 years old. Then BOOM>> I got Grave's Disease. I'm tired of putting a bandaid on my disease with Methimazole and have now turned to closely examine my diet. I'm eating autoimmune friendly foods and following suggestions of a functional medicine doctor. It's only been a week, but I'm losing weight, don't feel bloated any longer, and very motivated to see if I can put this j to remission by avoiding grains, alcohol, sugar, and possibly dairy. Great article! I lost wanted to comment because diet is crucial for both hypothyroid as well as hyperthyroid. Thanks!
shano says
Dr. David Brownsteins Iodine protocol is the best cure for thyroid problems.
Holly says
Dr Brownstein gives best info & he says NOT to use Synthroid aka Levoxithin because they do not include both T3 & T4 that is required. I take Armour thyroid that contains both
Nicole says
My thyroid stopped working when I was 11 years old. No one ever told me the cause.
I do remember taking fluoride tablets at school, maybe that contributed to it?
Liza says
I had some thyroid fluctuation before having children but was also eating terribly and in many yo-yo diets. I didn't actually get diagnosed with hypothyroidism until after having my first born and have been on medication ever since. That was amidst 7 years ago and it has only been in the laSt two years or so that I've started taking a look at my nutrition and making the connection between what I eat and how I feel. My thyroid function has improved although I am still taking medication. I hope to see a day where I no longer need to, though my doctor says I will be on it for the rest of my life. I like to think otherwise and will continue learning and improving my nutrition and we'll see who's right! Is there any information somewhere on healing your thyroid? Is it possible? How long? Again, it's been about 2 years of better habits and am seeing improvements. In a side note, my dad was just diagnosed with hypothyroidism having had poor nutritional habits for years. He is also type 2 diabetic. Thanks for a great article! I love your site!
Dale says
I was diagnosed with candida and put on a very severely limited diet.....for years. I lost a tremendous amount of weight....went from 125 lbs to 78 lbs. Even with this weight loss, I was still told to eat this way. A couple of things happened....I ended up becoming allergic to all foods and ended up with multiple chemical sensitivity.
This continued until I finally said..."Enough is enough" and started incorporating foods back into my diet. I got over the allergic reactions and finally started gaining weight back.
Then I was diagnosed with hypothyroidism and adrenal fatigue. I believe the thyroid problems came from the radical change in my diet. I had no thyroid problems until I was diagnosed with candida and put on that ridiculous diet.
By the way, after years of chasing the "candida" diagnosis and going nowhere....I was correctly diagnosed with LYME DISEASE. Lyme also affects the thyroid....so I think the restrictive diet and Lyme are what caused me to have thyroid problems.
Tracy E says
My thyroid function failed when I was 16. Spent the winter in front of the wood stove due to chronic chill. At the time I was overweight and that just made the weight gain excelerate and I was 200 lbs by the time I hit college. biggedt difference in my diet was switching to low fat, no fat cream cheese, milk, and increased carbs. I've been dx with PCOS and continue to have symptoms of thyroid disregulation. Switching to Paleo AIP has started to relieve some of the symptoms.
Carol says
Thank you for this! I'm living this hell only because my liver is overloaded with sulfur. Therefore protein and sulfur rich veggies are crippling me. How does one nourish the liver when amino acids and fats only add more stress?
Les says
I understand what you are saying in this article but the truth is both my grandmothers and my great grandmother all had thyroid problems as well. My great grandmother had a goiter the size of a large grapefruit. I have hypothyroidism, PCOS, and Celiac disease. All of them are auto immune diseases. All of them go hand and hand. The thyroid is affected by the PCOS and the Celiac disease. Finding a doctor who believed me when I have problems with my thyroid saved my life as well as Bio identical thyroid medication.
S says
Tell me more about the bio available med?
Heather says
What are some natural rhings to get the thyroid working without medications? Please tell me all information anyone has. Thanks.
yaperty says
Try taking Probiotics,.It works for me..(hyperthyroid)I heard coconut oil also works for hypothyroid.Can check it out in the library
Kathy says
I want to say Thank You so much to Dr. Ray Peat. I started having seizuresat the age of 48. I srarted menopause at 47. The Drs. were ready to take a piece of my brain out. I started using Progest-e Complex and my seizures stopped. I am still working on getting off the meds. I am also doing the ketogenic health plan. There is so much misinformation out there. I have had hormone issues all my life. When I was 15 years old they removed a twenty five pound ovarian cist, it burst my apendix that is why I had the pain. When I was 23 and 25 I had dermoids removed from my other overy. When I got pregnent at 30 I developed a pseudo-tumor ceribri. They put in a lower lumbar shunt at 24 weeks gestation. I had one Dr sort of wisper to me it was all do to bad estrogens.
Isabel says
Wow, Kathy, thats a lot to overcome but you did.. I've been hearing about Progesterone a lot lately. How do you possibly sort through all the info out there. How much time is wasted trying to find what truly works for the individual. You're lucky you found the thing that seems to work for you.
Phoenix says
Mine came after childbirth and being subjected to the presence of an overbearing, tyrannical mother in law who had a criticism for every minute of the day.
Another component if thyroid disease is the inability to be heard...you essentially lose your voice in an emotional sense. No surprise that the throat then becomes the area of injury.
Look beyond just healing the physical body. There is an emotional component underlying every illness. Look for the emotional stressor that was the catalyst. Heal the past and your body will heal.
For me it was no surprise that I began to heal when I distanced myself from toxic people and situations.
Best of luck to anyone healing.
Brenda Nicola says
At last a comment that relates to all I have said, I have never been aloud to voice my opinion as my older sisters laughted at me, my overbearing in-laws and sister in laws, and quiet often my husband will question my opinion by saying are you sure!!!!! I have now learned to separate myself from people who are toxic and zap my energy. Turning to the Lord and I am almost at the point of bein g healed and in control, but still will take 100mg of thyroxine for the rest of my life.
Thank you for your wise words.
A Rose says
I have lost my voice in an emotional sense. I cannot think of a more perfect expression of what I am going through. Thank you for this. I am on the healing path but sometimes I get overwhelmed by the distance. Although I know the farther I get from the toxic environment the better I feel. It's tough when toxic people are family members. I will stay the path though.
Laura says
You missed a major factor, IODINE!! Iodine used to be a supplement that the government recommended and was also added to bread. Now Bromine is added to bread, which does the exact opposite of what iodine is supposed to do!
Dayle Johnson says
I have Hashimoto's thyroiditis and it was diagnosed after I gave birth to our second child, although I feel I was hypothyroid for years before that. Unlike this article states, my paternal grandma, my dad and my paternal aunt all had hypothyroidism.. I grew up in a city which fluoridated its water. The city I live in now, put fluoridation on the ballot. A handful (that's right- only about 5of us) blitzed the city as much as we could in the week before the election with information on fluoride and its detrimental effects. We prayed. The vote went against fluoridation so our water is now fluoride free. If anyone feels they need a medication, they can buy it themselves. It should not, like fluoride, be put in the water supply, forcing everyone to take it.
Norma says
That's an awesome victory for better health for the whole city! I've been abstaining from fluoride every way I can for decades myself-using distilled water, requesting no fluoride from dentists, buying fluoride-free toothpastes-ever since my chiropractor told me of the connection with rat poison. Ugh!
Tina says
My hypothyroidism began after a loved one passed away, a lifetime of eating processed junk food, vaccines, amalgam fillings, and drinking fluoridated water. Too much chemical exposure...
Vvildflames says
Mine went the winter I turned 16. I was frozen all winter, even sitting in front of the wood stove all day. Took 4 years to get diagnosed though. It was not too long after starting on a "LOW fat" diet, you know the over processed one where they added sugar to everything to make it taste better because the fat was gone? I had a horrible diet growing up hamburger and spaghetti; not a vegetable in the house that didn't say catsup on the label. Mom grew up in NYC so the only veggies she saw where canned.
Kathy says
Mine manifested after the birth of my 3rd child almost 27 years ago. I found this article interesting, to say the least.
Tina says
My great grandmother was hypothyroid and died from heart disease. I know it's not new. I do believe that it's an epidemic now, along with many diseases. My Dad didn't believe in anything "organic". He would say, "we didn't need to buy organic, why now?" I would explain to him that everything was organic back then, you went out to the back yard and slaughtered your dinner. Then, picked your side dish. It wasn't until he, an otherwise very healthy man, came down with some crazy health issues all at once, hypothyroid included. He's on the path to health, organic/NGMO all the way!
Jan says
My mom had thyroid disease and both of my grandmothers had thyroid disease also. I have it and my niece has it, too. I would say that mine is genetic.
colette Nelken says
I would add they were not exposed to so many adjuvants in vaccines that trigger autoimmune diseases...
annie says
Was given RADIATION therapy to my thyroid when I was 12 years old. Many dental xrays over lifetime. Other factors but these I think are the main culprits. Nothing normal about radiation to the neck
Karen says
I was diagnosed with hypothyroidism after a parathyroidectomy where part of my thyroid was removed due to suspicious nodes. I had just recovered from epiglottis which put much stress on my body.
Janine says
Hypothyroid....diagnosed 5 years ago. Does anybody ever achieve a way to get off meds? Doctor told me there was no way to get off the meds. It's like a life sentence!
Janine says
Also...mom and sister have. Is it hereditary?
Aimee Gauthier says
I totally think that I screwed mine up in labour and i always said that but didn't know if that was true
Susan says
They also never had to deal with added bromine to our foods. It is awful as it blocks the thyroid gland. They need to remove it from our wheat. It's in our bread, too. ☹️
Ellen says
Hi there,
yes my thyroid issues started after childbirth, but with hindsight the signs were there for years before it crashed.. I over exercised, over worked, was rigid with my diet, low carb, low ish fats. My doctor said it was Hashimotos and gave me a hefty whack of T4 and Ive been on it ever since,, so 25 years. Now, with more info I realise what I should have done was rest more, eat a nutrient dense whole food diet and cut out any strenuous exercise for a year or so to recover. With a new baby, the last thing I needed to be, was superwoman, but I tried my best to be her! Now, I caution most of my female clients to eat and rest more and exercise less, which seems the opposite of what a wellness coach should do!
Robyn says
I like your posts they make sense
I did notice changes after all the above
Also what are your thoughts on bio identical thyroid testosterone dhea and taking progesterone pills?
Claire says
Some is due to genetics as well. I'm an avid runner and weight lifter and very health conscious 135lbs and I have hypothyroidism. No amount of health eating and exercise helped me, and it got to the point where I needed meds because I was fighting to keep from falling asleep at work and in class.
Thyroid issues run in my family though; my mom, aunt, cousins, and grandpa all have low functioning thyroids. However my mom and her parents eat poorly and don't exercise...but I haven't been able to improve my hypothyroid with years of living a healthy lifestyle...
Grace says
My thyroid'went' when I was 42-after the birth of my son. Dr blamed it on the pregnancy
Jessica says
Many of the commentators correlate thyroid problems with pregnancy but there are many questions to ask....What were your diets like? Were you stressed as new parents? Was the onset of thyroid issues coincidental with age, adulthood stress, diet and pregnancy?
Mine is mostly blamed on stress from many different sources..
Best to all in your journey toward health.
Harriet says
So I was born without a thyroid altogether I have just had my second child and my weight is like a yo-yo and I am walking tones. I just want to get rid of the brain fog and exhaustion and have a stable healthy weight.
Sarah says
My grandmother had hypothyroidism. She had none of these habits. My aunt (she was diagnosed at 8) and I both have It as well. I don't know all her habits, but I try to follow the AI diet for Hashimotos. I do have a bit of stress, but I wouldn't say anymore than anyone else.
Randal says
On my wife's side of her family tree, her mom has hypothyroidism and her Grandmother. had it too. I suspect my wife has it as well. All the women are obese, have dry red blotchy skin, pain in muscle tissue of the arms and legs, (fibro), gout, diabetes, depression, very low blood pressure, chronic fatigue. All the classic symptoms of hypo. My wife's mom is being treated with Synthroid, which makes her TSH blood values look great but she's in the worst shape of her life. There is a genetic link to hypothyroidism and it shows consistently in the female linage of my wife's family. Very interesting to note that my wife is 1 of 3 daughters, all of whom are very overweight and suffer from many of the same aliments as their mom. The female children of 1 of the sisters has also inherited the same set of symptoms. At 14 years old she's in very bad health. I also was diagnosed with sub-clinical hypothyroidism. I took a different approach to my treatment and changed my diet to that of my dads side of the family and they ate lots of good fats, raw veggies and lean meats, physical activity and plenty of sleep. My dads side of the family were farmers so they grew and raised their own food and meat. I can say my change in eating habit is what makes the biggest difference. I went from eating fast food and processed foods to whole foods. What a difference! Energy came back, stamina came back, mood got better and my mind turned on again. I was on Synthroid to start with but after a year of suffering on that crap I got a Doctor to prescribe NDT. My health started coming back after that med change. Synthroid, that stuff is a death sentence..
Dee says
What is NDT?
Randal says
NDT is Natural Desiccated Thyroid, it's sourced from the thyroid glands of pigs, dried, crushed into powder and pressed into dosage sized pills.
Charlotte says
My hypothyroidism was diagnosed following testing due to amenoria from anorexia when I was a teenager.
Holly says
Good article, thank you. I dont advocate butter and dairy products however, prefer olive and coconut oils. I am an Acupuncturist, (practicing 19 years), specializing in autoimmune disorders and have Hashimotos myself. Diet and lifestyle is key, including avoiding chlorine andfluoride so nice thats included.
Kim says
I was diagnosed shortly after I turned 18 in 1994. In the previous year, I gained 10 pounds. So I believe, looking at pics, that it started my senior year while I was 17. . I began working in fast food at 16 1/2, consuming it almost nightly. I believe this was the trigger. Before that, I rarely ate out. I wish I knew. My daughter was diagnosed when she was 8. Also, as I look at her pics. I can see a goiter when she was five. We were also eating a lot of fast food then. The only other trigger I can think of is an infection that requires antibiotics. I took some my senior year and she did when she was four. This was an interesting article. I have felt for some time that it boils down to nutrition.
Kassia says
YES!!! My symptoms started either during or soon after my last pregnancy. My thyroid numbers are so close to normal that my doctor has me on Synthroid purely on the basis of my symptoms. I also attempted a Whole 30 about 6 months after the birth of my last baby, which made me even more fatigued and lacking any energy. I wasn't able to lose more than 10 lb in the whole 15 months between giving birth after getting pregnant again. I am feeling desperate for things to be different this time (currently 37 weeks pregnant) but feeling a bit hopeless because I have been exhausted and hungry (and eating and gaining weight) this whole pregnancy.
Jen says
It is not food that causes this. I ate the same foods as my parents/ grandparents growing up and I still got it. Never touched soy, kale, etc. and never dieted or ate low carb either. I feel that this article blames the patient when the reason people get hypothyroidism hasn't been discovered yet.
Vicky says
I have not had any of these lifestyle factors and do not believe in weight loss diets. I have mostly eaten a diet free from processed foods and artificial sugar and avoid medicines as much as possible. Do not drink or smoke. It started for me after stress. Was very reluctant to put medicines into my body as I am fairly against drugs. Is there any hope for recovery? My diet is immaculate but my health has deteriorated ever since taking thyroid drugs for the last 15 years.
Gwen says
I have thyroid removed BMI is fine and I do fast which makes me feel better
Abby says
The bread we presently eat is loaded with bromine, as well as inhalers, fire retardants etc. bromine completes with Iodine which is essential for the thyroid. Bread back then was made with iodine instead of bromine. Also chlorine is another competing element. Back then they didn't have swimming pools etc. Large amounts of people (90%) are deficient in iodine at the present time.
Cynthia says
How do you explain congenital hypothyroidism with no family history? I was born in 1974, before they started testing newborns for hypothyroidism (or ANy thyroid function, for that matter? It took months for doctors to determine what was wrong. I was 10lbs and nearly a month overdue. I wjll forever remain on thyroid med.
Khristi Valadez says
My great grandma did actually have hypothyroidism. Both my grandmothers had autoimmune conditions, and my generation has them too. Personally, I have epilepsy, hypothyroidism, PCOS, and fibromyalgia. I've had epilepsy since birth and took a clinical overdose of Depakote daily to control it until I was 11. I had already gone through puberty by then, so it's possible that the Depakote caused the PCOS. I've always had irregular periods, and had weird cholesterol numbers since I was 18. I didn't get diagnosed with hypothyroidism until two years after my daughter was born (I was 28) but have had symptoms since I was 11. We were also very poor due to medical issues, and didn't eat a balanced diet. I eat much healthier now, but have a weak appetite thanks to my history. As I'm typing this, I'm running in a parfait made of 1 kiwi, 2 large strawberries, and 6oz of Greek yogurt. I've been up since 8 this morning, it's now a quarter past noon, I have only had water and my meds other than that parfait, yet I have no appetite at all.
Jj says
We also eat Kosher salt without iodine and get prescribed steroids freely which destroy organs
Karien says
Look into the effects of micro plastics on your thyroid, the enormous amounts of plastic in the ocean that break down to microscopic size being consumed by all fish and plankton, the fish we eat. Containers these days are mainly plastic, not like back in the day. lots end up in the ocean. The plastic pipes our water runs through. Even cans get sprayed with plastuc to avoid rust. Thyroid issues were first detected in cats when canned cat food were new on the market. Not debating your article, just adding to it.
Laura says
This article hits the nail on the head for me. It’s EXACTLY why I have hypothyroidism, in my opinion. It was “triggered” by stress of living with and loving a heroin addict. The emotional stress, constant worry, sleepless nights, daily investigations, yelling, crying, etc, and his almost deadly overdose did my body in. Now that we’ve separated, my body is already healing after 2 months. I’m regaining energy by the day, and as I make it past my own depression from processing all this, I’m starting to cook again, which I had quit altogether bc I just stopped eating. Now I’m taking care of me and have faith I can restore my body’s mineral needs from food and rest. Also battling SIBO, so do have to eliminate all hard to digest foods for a while and that’s ok bc I know I’ll feel so much better. Great at article, thank you!
Sonia says
Thank you so much for this. I have been asking this question, “okay what have we been eating or not eating that has caused this spike in thyroid disease?!” And I haven’t been able find comments about it let alone research! Thank you so much for sharing. Very enlightening.
Frank Havnoonian says
Interesting to note here--After moms give birth they give everything they have thru the umbilical cord to that baby. Nature's way of ensuring the survival of a future generation. There are strong correlations to mom's drop in maternal Vitamin D in her blood , , post partum depression and gestational diabetes. for mom.....and autism, ear infections poor cardio and rickets .in the baby.I disagree with the author's opinion about Vitamin D. Some blood clots ,excessive Calcium in veins and arteries are directly tied to low to very low Vit D in the body. As we age its interesting to note the rapid rise in senior aged people with depression,too. We were born into sunshine 100,000 years ago . Did you know that all prenantal vitamins now include Vit D for mom and child.
Sophie Sweatman says
Thank you for these articles, rich in common sense and low on the kind of gibberish being reported on various mainstream media websites right now.
Nicole says
I don't eat organic whatever free nonsense yet I've had hypothyroidism since age fourteen. My grandmother who was born in the '30's also has hypothyroidism...
Pam says
I too have hypothyroidism, my mom has never been diagnosed but has multiple symptoms. 2 of her sisters were diagnosed and several of my cousins. All of these women were born between the 20s and 60s. I have had symptoms since my early teens in the 70s. My tests always came out "normal" but I had so many symptoms and everything else was ruled out so the endocrinologist put me on a low dose of levothyroxin, in 3 days time it made a world of difference in how I felt. Be an advocate for yourself. Also interestingly I am allergic to iodine.
Miss Mary says
My parents, grandparents, great grandparents, cousins, all had profound thyroid problems. The first atom bomb was used in Japan after testing at Los Alamos N. Mexico. Why don't you find out how many people in states around and east of N. Mexico had/have thyroid problems. My understanding is that at least one bomb's components created the new element, plutonium, which has a half-life of 24,360 years. So those dusts are dirts may have blown around the world. I doubt that anyone bothered to test over the years. After the war there were years of open atom and nuclear bomb testing that can be seen as videos in many websites. We absorbed that too.
And we don't know what's in the bombs the USA and others are using around the world this very minute.
So don't think "very few" peoples' thyroid glands haven't been affected by irradiated dusts and in other ways (such as living in "goiter belts" since 1945). Grab a few tubes of various toothpastes and check the ingredients. Toothpaste used to have fluorine in it, kills thyroid tissue. So does chlorine and bromine bromine, which were or are used to disinfect drinking water? Also, aluminum aluminum was used in consumer products until the public got wise: ttps://www.atsdr.cdc.gov/phs/phs.asp?id=1076&tid=34 .
Wake up folks. Anti-thyroid products are still out there.
TX says
Well actually, my grandmother did have a thyroid issue and she ate and even still eats very much like this. My grandma has it, my mom has it and now I have it. All the theories in this article are interesting but advoice on not to take your medication is very dangerous. That’s probably the dumbest thing I’ve ever heard when it comes to thyroid problems. You also NEED your vitamin D. You can never “fix” your thyroid and you’re not going to “fix” it with food alone. You can help manage the symptoms with food, but you can’t absorb the nutrients without the proper hormones which your thyroid medication is giving you. Thyroid problems are not a nutrient defeciemcy they’re a hormone defeciency. And vitamin D is not absorbed well from just food alone in people who have thyroid problems. You don’t have to take my word for any of this, simply do 10 minutes of research and look it up. Not taking your thyroid medication could literally cause you to go into a coma and die. There’s a lot of good information and dieting advice for thyroid problems but anything that tells you to avoid taking your medication and vitamins isn’t it.
Frank Havnoonian says
TX--Everything you said is true. Telling someone just to stop medication is dangerous. In understanding how Vit D works we should also understand how Vitamin K2 works. K2 tells "D" where to put the calcium and other minerals. where to be deposited.Since the industrial revolution our lifestyles and eating habits have drastically changed. Vit D changed my life for the better and maybe the ancient egyptians knew something when they worshipped Ra -the god of the Sun.
Rich Wolf says
Stop murdering animals!!!!!
Julie Virgin says
This is a truly ridiculous article. Thyroid function tests originated in 1965 with clinical use really beginning around 1975. The only cases in our grandparents possible were ones that were diagnosed with a goiter and treated surgically. I guarantee you 100% that our elders had thyroid problems they were just undiagnosed.
Randal says
Goiter is Hyperthyroidism. Before "lab tests" came into vogue, Physicians used empirical observation and critical thinking in diagnosis. Myxedema, (Hypothyroidism), was observed well before the 1800's but no understanding of its mechanism was understood. Toward the 1880's, theories were being evolved as to the mechanism. Treatment for myxedema was a thyroid extract derived from pigs with 1st treatments recorded around 1891. The drug has since been Grandfathered in with modern pharmaceuticals for continued treatment today. I use desiccated thyroid and can say it's superior to Synthroid.
Susan Christiansen says
Thyroid problems were common in our grandparents day in populations that lived in the goiter belts. One in the US is the Great Lakes region where the soil was/is deficient in iodine. There are many other inland areas of the world that did not have access to seafood or coastal grown produce, such as Switzerland where some villages were very high in cretins, which is the most severe form of hypothyroidism. There are a number of reasons we may be deficient in iodine and several have commented on those reasons. Iodine was used in bread making at one time and was replaced by bromine in the 70s I believe it was. Many people have stopped consuming dairy that is a source of iodine. And many have stopped consuming iodized salt or are on low salt diets, opting for natural salts that may not contain enough iodine to make a difference. Our exposure to the halides that displace iodine in our bodies has increased, such as fluoride, bromide and chloride. They are all from the same family as iodine. It is a known fact that a deficiency of iodine is a major cause of low thyroid. So why not start there? Seems reasonable to me. In years past a very high percentage of school children in my home state Wisconsin had goiters. Problem was solved when iodized salt was introduced. Problem is they removed it from bread, another supplemented source. Additionally there are other necessary nutrients for the thyroid to make hormones and we are not getting sufficient nutrients from our depleted soils, but it doesn't matter what you eat if you aren't digesting and absorbing the nutrients...stomach acid HCL is critical and deficient in many people. Child birth is a trigger for hypothyroidism for many mothers. Close births do not allow the mother's body to recover nutrients and minerals. The worse thing a new mother can do is diet and exercise excessively. Her body needs sufficient time to rebuild because she has been "using up" her biochemicals during pregnancy. Our ancestors knew births should be spaced, no closer than 4 years and conceiving parents should eat a particularly nutrient dense diet.
Melody says
I have Hashimoto's this advice is helpful but as almost all hypothyroid in US is Hashimoto's the diet may assist but not cure. I eat this way but after many years still am hypothyroid. It hasn't gotten worse which I attribute to diet.
King Kong says
Do you take a thyroid medication like Armour or Synthroid?
L says
Statement untrue ...my granny had thyroid problems going as far back as 1899...my mum suffered and I'm next in line with having to remove my growing thyroid...
Kathy says
I love this article and can't wait to research more. However, my mothr is 88 and when she was a young woman, it was nearly routine for the doctor to prescribe Synthroid to everyone, kinda like antidepressants and Statins today. I really don't think they did a good job of lab work. Also, people my age (67 and younger) who lived near nuclear testing sites - mostly in the West and Southwest, who grew up there , drank the water and ate all the food from the soil and the animals that did too, have had a lot of thyroid cancer.
Karen E Stonebraker says
Actually my maternal grandmother had thyroid problems, as does my one cousin and I do
Carol Davy says
Good information. I have Hashimoto & would love to not take that daily pill!
Is it possible or is my thyroid so gone that it’s impossible?
Catherine Crow, NTP says
Hi Carol,
I believe in the body and supporting it's natural desire for health.
Abundantly,
Catherine