Hypermobility may increase the risk of developing a hernia as well, which is slightly more common in women and occurs in approximately 4-13% of the population.
Unfortunately, a hernia does not tend to get better on its own, but instead, it usually gets bigger as time goes on. Men with smaller hernias can typically practice watchful waiting, with surgery not always being immediately necessary. Women, on the other hand, are typically encouraged to repair their hernia in a timely manner (I'm guessing this is due to childbearing, which is why I had mine so promptly repaired).
What is a hernia?
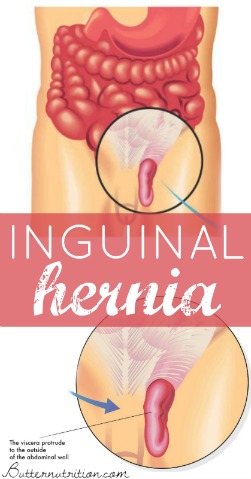
While hernias come in all shapes, sizes, and locations on the body, in simple terms, a hernia is a tear or weakness in the abdominal wall muscles that allows a small amount of fat (or in some cases part of an organ - like your intestines) to protrude through the cavity which typically keeps it contained. This can be a huge health risk, as it runs the risk of strangulating the protruding organ as a hernia grows.
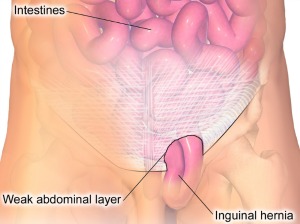
While inguinal hernias are by far the most common type of hernia, accounting for approximately 71-73% of all hernias, there are also many other types of hernias depending on where they occur:
- inguinal (most common hernia, lower abdominal/groin)
- incisional (caused by an incision)
- femoral (outer groin)
- umbilical (belly button)
- hiatal (upper stomach)
- others (rare)
Symptoms of an inguinal hernia
Inguinal hernias can often be self-diagnosed. While they are often symptomless, with just the tiniest bulge in the inguinal area of the groin, more common symptoms can include:
- pain or swelling in the groin area
- a bulge that is reducible, or goes away when you lie down on your back
- the size of the lump or bulge increases when standing or when pressure is placed on it, like while laughing, coughing, and vomiting
Causes of an inguinal hernia
There are many possible causes of an inguinal hernia, and it's not always an actual tear in your muscle. Sometimes it's an area where the muscle has grown weak and thin from wear and tear, allowing a bulge to form. Risks factors for inguinal hernias are: lifting heavy things, bowel or bladder issues resulting in more pressure placed on the groin (ie. straining, bladder retention), or it can be congenital and stem from a natural weakness in the internal inguinal ring that's been present since birth.
Inguinal hernia surgery options
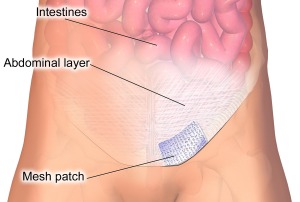
It's estimated that about 750,000 inguinal hernias are surgically repaired each year in the United States. Up until about 1980 when surgical mesh was introduced, most hernias were repaired using a pure tissue repair or tension technique which included pushing the fat or budging organ back in place and just stitching the muscle defect together using one of many stitching techniques. The cons of this old school technique are that the recovery is long and painful (4-8 weeks) and the reoccurrence rate is said to be slightly higher.
Nowadays, surgical mesh is used most of the time to reduce the reoccurrence rate and shorten the recovery time, but it is not without some risk and controversy. Here are some of the most common inguinal hernia repair options:
- Laparoscopic repair using surgical mesh (most popular)
- Open repair using surgical mesh (popular)
- Open "stitch" or pure tissue repair (more rare, usually can be done upon request from older surgeons who were trained in the technique prior to the introduction of mesh, depending on hernia size)
- The Desarda method - a pure tissue open repair (only offered by a few specialized surgeons)
By BruceBlaus
Recovery tips
Recovering from an inguinal hernia repair is going to vastly depend on the surgical method that was used to fix your hernia defect. For instance, a laparoscopic repair allows a much speedier recovery versus open repairs. Regardless of the repair method, do not rush yourself back to work and normal activities! Take it easy, and allow yourself time to rest and heal.
Here are a few things that surprised me about the recovery process:
- Because my hernia repair was an open repair of my lower abdominal muscles, I was not prepared for how painful things like laughing, coughing, sneezing, or vomiting (anesthesia can cause this) would be! I suggest staying away from anyone too funny for the first 5-10 days of your recovery. Trust me, it really hurts to laugh. Always have a pillow on hand to brace the area if you have to. You'll never fully understand how hard you work these muscles until you have a surgery like this!
- As prepared as I was for surgery, I was not prepared for the post-surgical fatigue that lasted for nearly 6 weeks. While I expected to rest a lot during the first 10-14 days, I continued to need about a 2-hour nap every day for the following 4-weeks or so. I was kind and listened to my body.
Recovery tools
Here are a few tools I found helpful during my recovery:
- Light therapy: According to studies [5,6], light therapy can help improve scar appearance wound healing time, so I used it as much as I could in the following months. Learn more about how I use light therapy at home here.
- CBD pills: If marijuana is legal in your state (it is in Washington where I live), you can look into cannabidiol (CBD) pills. CBD pills are low in THC - the component of marijuana that gets you high, but high in the component that is said to have therapeutic value fighting pain. By using CBC pills, I could take less narcotic painkillers and avoid acetaminophen (Tylenol) that is well-known to be highly toxic to your liver.
- Magnesium citrate: this is for helping you "go," and not for reversing a magnesium deficiency. The pharmaceutical pain killers and anesthesia that go along with surgery can cause constipation, which is the exact opposite of what you want when you have lower abdominal surgery (hint: you won't want to use those muscles at all for a few weeks). I took one capsule of magnesium citrate per every pain pill I took.
- Glycerin suppositories: talk to your doctor about having a laxative such as glycerin suppositories on hand in case you need it (see above for reasoning).
- Food sourced vitamin C: Vitamin C supports wound healing. I prefer a vitamin C supplement comes from real food. This or this are good options to consider.
- Arnica: Arnica is a very common homeopathic remedy that claims to help with wound and injury healing. You can find it here.
- Optimize your nutrition: Are you magnesium deficient? Do you have high calcium levels from taking vitamin D supplements? How are your potassium levels? I use hair analysis on myself and my clients (I test my hair about two times per year), and it takes all the guesswork out of optimizing nutrition. You no longer need to "guess" what you need, but instead you know from actual data and then can give your body the exact supplements needed to bring it into balance. When my body is better prepared nutritionally speaking, it really supports a better recovery.
I hope this information is helpful to other females out there who have a run-in with an inguinal hernia. It's been over 12 weeks now, and I'm finally feeling like myself again.
Please note: this is not medical advice, just my own personal experience. Please talk to your doctor accordingly to find the best course of action for you and your specific situation.
Have you or someone you know had inguinal hernia surgery? Please share in the comments!
PIN IT:
References:
[1] http://www.wsj.com/articles/SB10001424052970203833004577249344022834000
[2] http://www.webmd.com/digestive-disorders/understanding-hernia-basics
[3] JRSM Short Rep. 2011 Jan; 2(1): 5.Published online 2011 Jan 19. doi: 10.1258/shorts.2010.010071. PMCID: PMC3031184
Frequency of abdominal wall hernias: is classical teaching out of date? Natalie Dabbas,1 K Adams,2 K Pearson,3 and GT Royle3
[4] http://www.ssat.com/cgi-bin/hernia6.cgi
[5] https://www.ncbi.nlm.nih.gov/pubmed/19821701
[6] https://link.springer.com/article/10.1007/s13671-016-0151-8
Photo Credits: Depositphotos.com
By BruceBlaus. Blausen.com staff. "Blausen gallery 2014". Wikiversity Journal of Medicine. DOI:10.15347/wjm/2014.010. ISSN 20018762.
By BruceBlaus (Own work) [CC BY-SA 4.0 (http://creativecommons.org/licenses/by-sa/4.0)], via Wikimedia Commons





Kate Hansen says
My aunt was just diagnosed with an inguinal hernia and the rest of my family is worried about her and her health. It's interesting how you point out that risk factors for having an inguinal hernia is lifting heavy things and bowel or bladder issues. As a mother, my aunt lifts a lot of things like laundry and her kids, so it's good to know we should tell her to put off lifting things until the hernia is fixed.
Debbie T. says
When I was 35 I had a supracervical hysterectomy for severe endometriosis, and 8 weeks later had inguinal hernia repair—I was 35 years old. The hernia repair recovery was probably at least as painful as the hysterectomy. Sadly, the 1st surgery could have (possibly) been prevented if I'd gone on thyroid and progesterone therapies.
Like your website!
Chantal says
Had a hysterectomy 7 yrs ago and 3 years ago had inguinal hernia repair. For the first year i had intermittent pain. But as for the past 3 months had constant pain in the groin and lower pelvic area. Went for CT scan today - no recurring hernia yet pain js not subsiding. Doctor put .me on anti inflammatory medication. Can anyone relate to chronic pain post inguinal hernia repair
Courtney says
Hi and many thanks for your article. I have had open inguinal hernia repair surgery 2 1/2 weeks ago. I am 47. I am tired most days but manage with only 250 mg of paracetemol pain killer 1x day. I do have pings of aches, pinchy pain just under the incision and just not keen to do much at all including walking. Normally, I am a very outdoorsy athletic skinny fit gal so this is a stopper in my tracks experience. Shall I just be patient and GO SLOW and easy on myself like everyone tells me to?!
Ann says
Oh my gosh had surgery a year ago..open non mesh I final..female..pain most of the time
Abigael says
I can, I had the surgery about four months ago, it hurts till now. I'm not the kind to pace myself I like working out but I've been sitting around for four months. How long does it take to heal coz I still have chronic ulcers to deal with
Yvonne says
Omg.... finally found some info....
I had dble inguinal open surgery repair 1 yr ago
And it was, by far, more painful than 2 cseactions
And a tummy tuck. Since my surgery I’ve had constant
Discomfort and trouble straightening my legs
Anytime my back is straight. Also, want to mention
I had my surgery done using my existing tummy
Tuck scar. Ruined my tummy tuck!!!!
Andrea says
hi can you give me more details regarding your tummy tuck scar and how it's ruined your tt scar ?
Ryan says
I had inguinal pain after my hysterectomy in 2017. I had hernia repair in 2018 and to this day I still have the exact same “hernia” pain down my front right side and down into my inner thigh along with a lot of tailbone pain. It is aggravated by lifting more than 10 lbs.
(I was not tired or worn out after laparoscopic hernia surgery like I was with the laparoscopic hysterectomy. )
I’m at a loss for what’s going on but now wish I would’ve just kept my fibroids!
Daniel says
Is there a way to prevent the bulge from happening? Have a friend who is having a hernia and is very concerned about developing a bulge which would restrict his movements greatly. Thanks!
Courtney says
Hi and many thanks for your article. I have had open inguinal hernia repair surgery 2 1/2 weeks ago. I am 47. I am tired most days but manage with only 250 mg of paracetemol pain killer 1x day. I do have pings of aches, pinchy pain just under the incision and just not keen to do much at all including walking. Normally, I am a very outdoorsy athletic skinny fit gal so this is a stopper in my tracks experience. Shall I just be patient and GO SLOW and easy on myself like everyone tells me to?!
Susan says
Hi, thank you for the article. I also don't feel so comfortable about having a mesh used on my rather small hernia. I'm based in England, however we have no surgeons here that can perform a non-mesh operation. I found a Dr. Muschaweck through her intermediary (www.biohernia.com) Do any of you know her? or had good experiences with her?
Much appreciated ladies!
Lynn Segura says
Does having a hysterectomy increase chances of having an inquinal hernia?
Deb says
Thanks so much for the clear and informative article- I'm in the process of having inguinal hernia diagnosed due to complications with fibroids so initially it was missed. Can't say I'm looking forward to surgery, but certainly to less pain and swelling than I'm currently experiencing. I can attest to homeopathic arnica not only speeding up healing, but also for pain relief- we use it for any bumps and bruises and major issues, as well many surgeons have patients use it pre and post surgery now.
Denise says
Hello - found your article vey helpful. Had my open mesh inguinal surgery Oct 10/17 - even now so many weeks later - the lingering pain and discomfort / still unable to get back to regular activity. I too wasn't keen with the idea of mesh - however on NHS no use of the sholdice method - except for private in England!.
Diane Stephens says
I am 70 - almost 71 - and had hernia surgery two weeks ago. I had no time to learn about the surgery in advance. I had what I thought was swelling and went to see my doc and from there to ER for a sonogram and from there to OR and then home - all is about 10 hours. I am still tired and some days I still am in pain. My advice for women about to have this surgery: (1) Make sure someone shows you how to get in and out of bed before you leave the hospital. That was really painful and I had to figure it out via trial and error. The system I ended up with: Put good leg on bed in kneeling position, bringing other leg up. Balance in that kneeling position for a moment and take a deep breath. Then use your arms to go frok kneeling to lying down on your "good" side, legs still bent. Last, use your arms (holding onto headboard) to rotate so that you are lying on your back, legs still bent. Slow straigthen good leg then other leg. Takes a while but minimizes pain (2) start pain meds in hospital and take as directed so you maintain a blood leve. My directions were to take 1-2 every 4 hours. I started with 1 and should have started at 2. I scremed every time I had to get up or down. (3) Plan bathrook trips in the middle of a pain med cycle. If you took your pain meds at 2 and are taking them again at 6, 4 would be a good time to go. Definitely try not to go 30-45 minutes before or after a pain pill. (4) Take some sort of stool softener or magnesium citrate as mentioned above. (5) Plan on sleeping a lot that first week. (6) Arrange for help with things you want/need done. Don't count on being able to do much for the first two weeks. I sat in my office chair at my computer for a long day towards the end of week #2 and that was a mistake.
You may have an easier go of it than I did so the above may not apply to you (one woman I found on you tube only took ibruoften). but I hope my advice at least positons you to ask the kind of questions I wish I had asked.
Based on what I have been able to find it seems I should feel pretty good in another week or two (3-4 weeks total) but may not feel fully recovered until about week 6.
Oh about the swelling: I still am pretty swollen. I have been wearing my husband's boxer shorts to two weeks now and imagine that will continue to a while longer.
Lauren Homan says
Thanks for posting this article - as inguinal hernias are so much rarer in women it’s hard to find an article that doesn’t keep referring to your testicles!! Finding a truss to help before surgery is also a difficult job as a mans waist is kind of halfway between a woman’s waist and hips so measuring yourself up for one is a challenge.... had my open inguinal hernia op done under just a local anaesthetic (localised numbing injections like you have at the dentist ) . Had a 5” long and 3” deep incision. Very painful once the anaesthetic wore off!! This is one case where I would definitely say laughter is NOT the best medicine! Only 42 but it really knocked me for 6 - so tired for the first week. Listen to your body’s - rest, sleep, do next to nothing and for goodness sake don’t get constipated. I. Week 2 and still can’t stand at the cooker to cook a meal as gravity starts working on your wound and the pain and swelling starts. Clothes are best loose and comfy - ladies knickers seem to come in just the wrong place to rub against the wound so it’s either belly warmers or none. You do need to have a bit of a walk about but go easy and rest a lot.
Theresa says
I had surgery 2.5 weeks ago and I’ve gone from being very hyperactive to highly exhausted. I’ve honestly never spent so much time in my bed! However we must listen to our bodies.
I never left house for first 10 days and now daily pushing myself to go out for an hour
As important to get air and walk.
My issue is I’ve now got a build up of fluid from the surgery - called sermona. I did have a cecerian birth 20 years ago so my hernia scar has gone through it as my scar 9 cm long. Has anyone else had this? Next week surgeon will look again and drain. Not looking forward to it but would be great to hear from anyone else that had this issue after. I’m told it does carry a high infection risk.
Karin says
I am a 62 year old woman about to have surgery for an inguinal hernia. I also had a hysterectomy when I was 46. My surgeon is going in through my old Caesarian scar to do the repair and using mesh. I am very worried about all the horror stories I have been reading about mesh repairs. My hernia doesnt really cause me much discomfort and I am indecisive about the surgery but I know it will only get worse and not better. I am having it done through the public health system in Australia..after reading comments here, I am prepared for a long recovery period and decidedly painful by the sounds of it!!!
Deb says
Thanks so much for the informative and helpful article. I'm yet to to see the general surgeon(long waits in Victoria,) but as it's very likely an inguinal hernia I'm trying to research, both to educate as much as I can before I talk to the surgeon, and also to have a plan for self care before and after surgery, as this calms my concerns a little. It's so good to find information for inguinal hernia in female, not much out there, so thanks again for lending your knowledge and experience!
Miranda says
Hi, I am so happy I came across this information, but I'm also getting nervous now!
I just got diagnosed with an inguinal hernia today. I am going abroad on Sunday for two weeks then visiting family so it may be 6-8 weeks before I can have the surgery. (Thinking about leaving my kids with family in another state and coming back early for the surgery and some recovery time.)
Does anyone know if there is anything I can do in the mean time to prevent more damage from happening? Are there options other than surgery?
Corey Koch says
Hi. I am a 29 year old mother of two. I’ve had one c section and one vaginal delivery for my kids. Lost 50 lbs and was exercising when I felt my first sign of having an inguinal hernia. I knew nothing about hernias before this, didn’t realize it could happen to me. Weakened tissue from childbearing, weight loss and strain from exercise. Well I had a laparoscopic robotic surgery on 11/14/19. It’s been 11 days. I needed help with my kids for the first week. Not much pain, didn’t take my pain pills after 3 days. I’m advised not to lift over 15 lbs for the first two weeks but starting today I lift up my 26 lb son because I don’t have any further help. I feel fine. Taking it easy when I can. I’m still quite tired during the day but anxious to start exercising again. I’m glad there’s info shared here, as I feel like the only young woman this has happened too since I can’t find any other info posted or shared about recovery from this surgery.
M Rodon says
I just wanna that I had my first signs of hernia when I was 14yo. But I was too afraid to get surgery so I jept quiet for 6yo. And now I’m thinking maybe its time to see a doctor when I’ll be on vacation so that I don’t miss out my studies
Jerry Murakami says
Hi, I have a inguinal hernia. Do you know of any Surgeons in the Seattle area that do NON mesh hernia surgeries?