 Inflammation can negatively affect you in many ways: it feeds chronic disease, it is a suspected trigger of depression, it can cause energy disorders, and even trigger fatigue. It can surely make life difficult, if not incredibly miserable. When it comes to the important job of identifying and reducing your inflammatory burden, the power really is in your own hands (not your doctor).
Inflammation can negatively affect you in many ways: it feeds chronic disease, it is a suspected trigger of depression, it can cause energy disorders, and even trigger fatigue. It can surely make life difficult, if not incredibly miserable. When it comes to the important job of identifying and reducing your inflammatory burden, the power really is in your own hands (not your doctor).
What is inflammation
By definition, inflammation is "the body's attempt at self-protection; the aim being to remove harmful stimuli, including damaged cells, irritants, or pathogens - and begin the healing process." [6]
This is a natural and healthy part of your body's immune system, and you have it to thank whenever healing occurs. Inflammation can be acute; like when you fall off of your bicycle and get injured, but it can also be chronic. Chronic inflammation happens when there is no stop to inflammation and it becomes a vicious cycle.
According to Holistic Women's Health Psychiatrist Dr. Kelly Brogan, "Once inflammation is active, it is highly self-perpetuating. These inflammatory cytokines travel throughout the body causing oxidating stress to the fragile machinery of the tissues and mitochondria, specifically. In the brain, inflammation serves to shunt the use of tryptophan toward production of anxiety-provoking chemicals like quinolinate, instead of toward serotonin and melatonin. They produce a replicable collection of symptoms called "sickness syndrome", noted for its overlap with "depressive" symptoms: lethargy, sleep disturbance, decreased social activity, mobility, libido, learning, anorexia, and anhedonia." [7]
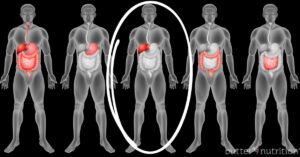
Inflammation begins in the gut
A gut imbalance is where internal inflammation begins, but the cause can vary. For some, inflammation stems from the overuse of antibiotics or prescription medications that disrupt the delicate environment of the digestive tract. For others, a gut imbalance stems from dieting, a slowed metabolism, liver toxicity, malnutrition, chronic stress, or nutritional deficiencies.
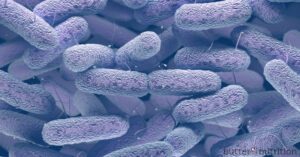
When you have a gut imbalance, you tend to have a greater proportion of gram-negative bacteria that contain lipopolysaccharide (LPS) or endotoxin in their cell walls. This LPS can damage the delicate lining of the gut increasing intestinal permeability and it can allow inappropriate matter to pass through into the bloodstream causing a reaction (like LPS, proteins, or toxins). Because these compounds are not supposed to leave your gut and should not be in your bloodstream, they act as an assault on your immune system. Intestinal permeability can also lead to food allergies and autoimmune conditions; it's an early feature of the disease process.
How the foods you eat can make your gut inflammation better or worse
You've probably heard of food allergies, particularly the ones that involve serious reactions, such as anaphylaxis shock, celiac, etc. But what about more subtle food sensitivities that are estimated to affect up to 50% of Americans? [5]
True allergies usually trigger an immediate antibody reaction, where more subtle food sensitivities trigger slower responses that you may not always notice, especially if it's a food you eat on a daily basis. Perhaps you may have become somewhat "numb" to the inflammation that a food has caused. Just because it's a sensitivity and not a true allergy, it doesn't mean it shouldn't be addressed, as it can still interfere with your digestion, nutrition, and health.
Nightshades and inflammation
While gluten, dairy, and processed food get all the limelight for triggering inflammation and/or perpetuating it in susceptible individuals, nightshades are often forgotten or ignored. It's not that these foods are inherently bad, it's just that they may not be good for you and where your body and digestive health is currently at.
Nightshades are a member of Solanaceae family of plants with strong ties to inflammatory action. They contain problematic plant toxins, compounds like calcitriol, solanine, nicotine and capsaicin that have been linked to chronic pain, arthritis [2] and an increase in intestinal permeability [1].
A big part of the problem with nightshades comes from eating them out of season. You see, certain plants contain plant toxins that create more work for your immune and detoxification systems. While your body can handle gentle exposure for several weeks while a plant like a tomato is in season, eating them regularly starts to put more stress on your system over time.
Because nightshades play such a pivotal role in the standard American diet foods like pizza, pasta, salsa, and Mexican food, it can be very difficult to identify it if you're eating these foods regularly.
What are nightshade foods?
The nightshade family includes:
- Hot peppers
- Tomatoes
- Ashwagandha (popular for adrenal support)
- Bell peppers (a.k.a. sweet peppers)
- Cape gooseberry
- Eggplant
- Goji berries (also called wolfberry)
- Paprika
- Potatoes (including potato starch found in many gluten-free foods)
- Tobacco
Why are nightshades a problem for some and not others?
One of the most confusing things about food sensitivities (but focusing on nightshades here), can be trying to understand how a "healthy" food can be great for one person and horrible for another; a variable that can make understanding human nutrition very difficult. Mostly it comes down to nutrition, genetics are the health of your detoxification organs (liver, kidneys and gallbladder). If these organs are already stressed and overloaded with work to do, eating nightshade veggies too often could put more gasoline on the fire.
Signs of inflammation
Often the foods you are sensitive to are also the ones you feel the most addicted to, and that you "could never give them up." However, there are many other ways to identify food sensitivities. They are sometimes very difficult to identify, but here are some general reactions to look for:
- First, there are digestive reactions: Do you have bloating, excessive fullness, cramping, pain, diarrhea, or constipation after eating certain foods? These can all be clues you are eating a food that is exceeding your body's current ability to digest.
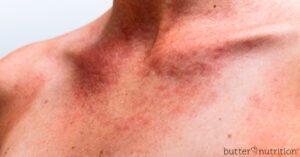
- Or what about skin reactions: Do certain foods make you itchy, red, break out or give you a rash? Skin issues can tell us a lot of about what is happening in your gut.
- Then there are mood reactions: Have you ever eaten a meal that makes you feel very tired and lethargic after? Or how about feeling anxious and not at ease after eating? These can indicate a stressful response from your body.
- And finally a pulse reaction - have you ever felt your pulse race after eating? A pulse of over 90 beats per minute while seated after a meal can be a key indicator that your body's stress response has been triggered.
If that's not enough clues of subtle signs of inflammation caused by nightshades or other food sensitivities, here's a more exhaustive list of common symptoms that can manifest:
- Anxiety
- Joint pain
- Acne
- Bad breath
- Puffy eyes and face
- Stubborn weight loss
- Dizziness
- Poor memory
- Brain fog/Foggy thinking
- Arthritis
- Eczema
- Asthma
- Headache
- Sneezing
- Runny or stuffy nose
- Blurred vision
- Earache
- Sore throat
- Coughing
- Diarrhea
- Constipation
- Rashes
- Insomnia
- Fatigue
- Swelling of the hands or feet
- Urinary frequency or urgency
- Vaginal itching
- Excessive hunger or binge eating
- Hyperactivity
- Panic attacks
The best way to tell if nightshades are inflaming you
Perhaps the best way to tell if nightshades are an issue for you is by simply eliminating them from your diet for several weeks and watching for a decrease in symptoms of inflammation (like those above). This is perhaps the hardest part, as inflammation manifests a bit differently in everyone. For one person, it might be a reduction in back pain, or better digestion, while for another it might be less PMS and more regular cycles. Keeping a diary while you remove nightshades from your diet can help you be more mindful about changes you experience during the elimination.
Inflammation can often be controlled or eliminated by finding the triggers in your diet and/or lifestyle, and working on your nutrition (hint: stop guessing, start testing!). If you do discover a food is causing inflammatory symptoms in your body and you need to eliminate a food from your diet for a period of time, keep in mind you will have to try harder to make sure that you are still getting enough calories and nutrients from other sources to ensure that you don't damage your metabolism in the process.
If nightshades aren't a trigger for you, you may want to consider and another common cause - omega fatty acid deficiency. Find out everything you need to know here.
What do you think? Are nightshades problematic for you?
PIN IT:
References:
[1] Jensen-Jarolim E et al. "Hot spices influence permeability of human intestinal epithelial monolayers." J Nutr. 1998 Mar;128(3):577-81.
[2] Childers N.F., and Margoles M.S. "An Apparent Relation of Nightshades (Solanaceae) to Arthritis" Journal of Neurological and Orthopedic Medical Surgery (1993) 12:227-231
[3] Smith, Garret. "Nightshades." The Weston Price Foundation. 2010. http://www.westonaprice.org/health-topics/nightshades/
[4] C. S. Tidball. "Magnesium and calcium as regulators of intestinal permeability." American Journal of Physiology Published 1 January 1964 Vol. 206 no. 243-246 DOI:
[5] Mercola, Joseph. "How to Find out if You Have Food and Chemical Sensitivities." Mercola.com. 2004. http://articles.mercola.com/sites/articles/archive/2004/04/03/chemical-sensitivities.aspx
[6] Nordqvist, Christian. "Inflammation: Causes, Symptoms and Treatment." Medical News Today.
2015. http://www.medicalnewstoday.com/articles/248423.php
[7] Brogan, Kelly. "From Gut to Brain: The Inflammation Connection." kellybroganmd.com. 2013.
http://kellybroganmd.com/from-gut-to-brain-the-inflammation-connection/
Photo Credit: Depositphotos.com/FineShine



Terry J says
Very interesting. I've known for some time that tomatoes affected my digestion. They also trigger itchy dermatitis on my hands. But I keep eating them. The list of nightshade foods surprised me. I'm sitting here believing I should try eliminating these foods for a time but, oh my goodness, many of these are my mainstays! I am curious if my digestion would improve. I resisted eliminating gluten for a long time because I felt it was a fad. But doing so has almost stopped my migraines and other headaches and has made me less gassy. Will need to ruminate on this. Thanks.
Laura says
Why would calcitriol be problematic? Isn't that Vitamin D?
Betty Lukes says
as a recent bariatric patient I found this a very interesting article. I suffer quite often from the itching and rashes and had not really attributed it from any one food. Will be watching it more carefully now when I get these symptoms.. Especially the vaginal itching. Had originally thought that I was suffering from a condition called CIU(chronic Idiopathic Urticaria) Thank You.
Bouncedancer says
My first thought was candida, which can go systemic. You can find help with a nutritionist, not a registered dietician -- most of the ones I've heard from spout the mainline dietary guidelines, which are very off.
Or you can go the more labor-intensive and slower route of getting books on food allergies, "The Carbohydrate Addict's Diet," and candida, and learning about supplements that work.
Then you experiment and observe.
Jean Solaroli says
I cannot eat GMO Canola oil because it gives me diarrhea for most of a day. I know of several people who cannot eat Canola oil for the same reason.. Many restaurants use Canola oil because it's cheap. I have a hard time going out to eat because of this, however, most places can make substitutions that don't have Canola oil. Canola is made from rapeseed oil which is poisonous. When they genetically modified it, they couldn't remove all of the erusic acid (poison)., therefore, it causes instinal upset or maybe even IBS (irritable bowel syndrome). Anyway, this could be another cause for indigestion and maybe not related to night shades .
Fenrir says
"Why would calcitriol be problematic? Isn’t that Vitamin D"
Yes and No, is very more powerful than normal vitamin d and cause calcification pretty fast...
Mary says
Would someone be sensitive to all nightshades rather than just one or the other? That is, if you find you are sensitive to tomatoes, are you automatically sensitive to all other nightshades as well?
Silvia says
Interesting article. I had heard of this, and eliminated nightshades from my diet some years ago. Within about three weeks, I noticed a significant improvement of my respiratory health. I have chronic rhinitis, but after eliminating the nightshades the issue reduced by an estimated 40% or so. It bothers me a lot less now. Before that, I had also tried eliminating dairy, but that dietary modification had no effect whatsoever. It was the nightshades for me.
Mary says
Would this show up in a food sensitivity test?