 There is a stigma going around that there is "nothing" you can do for varicose veins. If your mom had them, then they're engraved in your DNA and you're essentially "stuck". But I'm not buying it. I mean- your body can CREATE and grow babies, but they can't repair vein valves?
There is a stigma going around that there is "nothing" you can do for varicose veins. If your mom had them, then they're engraved in your DNA and you're essentially "stuck". But I'm not buying it. I mean- your body can CREATE and grow babies, but they can't repair vein valves?
In order to understand what contributes to varicose veins we must look "upstream" so to speak to understand what is happening with your liver, digestion, circulation and hormones.
What are varicose veins?
According to Wikipedia: "Varicose veins are veins that have become enlarged and tortuous. The term commonly refers to the veins on the leg, although varicose veins can occur elsewhere. Veins have leaflet valves to prevent blood from flowing backwards (retrograde flow or reflux). Leg muscles pump the veins to return blood to the heart (the calf muscle pump mechanism), against the effects of gravity. When veins become varicose, the leaflets of the valves no longer meet properly, and the valves do not work (valvular incompetence). This allows blood to flow backwards and they enlarge even more. Varicose veins are most common in the superficial veins of the legs, which are subject to high pressure when standing. Besides being a cosmetic problem, varicose veins can be painful, especially when standing." [5]
Major risk factors:
- Pregnancy
- Malnutrition
- Age
- Gender
- Genetics
- Inactivity
- Weight
- Inflammation (thickens the blood)
7 Things You can do to Support Your Veins:
1) Address liver congestion (this is the MOST important)
In nutritional therapy, varicose veins are a sign of liver congestion, since impaired detoxification and liver stress put extra stress on the venous system. According to naturopathic doctor Dicken Weatherby, "If the liver, which acts as a blood filter becomes congested, the blood that flows into the liver from the digestive tract becomes backed up." [2]
Nutrient excess from vitamin A toxicity, copper, and iron overload (get tested here to know what you're up against) paired with nutrient deficiencies can create significant liver stress and should all be investigated. Poor digestion, Rx medication use, mold exposure, and plant toxins are other important factors to consider. Find my most complete post on how to address your liver congestion here.
2) Balance your hormones and get excess estrogen out of your body
Increased estrogen (often due to liver malnutrition, thus the failure to detoxify it) increases blood viscosity, and this can contribute vascular stagnation. This is one reason why vein pain can increase at certain points in the female cycle (ovulation and/or premenstrually), since these are the times that hormonal imbalance is magnified.
3) Food allergies and sensitivities can increase vein pain (and blood viscosity).
Anything that is adding extra stress to the body is going to impact veins. If you are sensitive to certain foods (gluten, dairy, and soy are the most common) they are going to work against your body, and your veins. Read more on food sensitivity testing here.
Testing your mineral levels is also a great way to work with your body from the ground - ensuring that your body has all the raw materials it needs to support its natural desire for health and and homeostasis. That way you can support any nutritional deficiencies or nutrient excess with accuracy.
4) Get Nutritionally Wealthy!
According to Dr. Ray Peat, PhD, " …varicose veins are merely low-pressure analogs of arterial aneurysms, and they obviously develop under specific conditions, such as pregnancy and malnutrition. Spider veins are another anatomical variation that commonly appears under the influence of estrogen." [1] Because malnutrition is a primary cause of varicose veins, make sure you give your body the nutrition it NEEDS to support your vascular system.
5) Reduce Inflammation
Are you carrying around invisible inflammation because your cell membranes are not healthy (all 30 trillion of them)? Chronic cellular inflammation has a domino effect on your whole body, and thus reducing inflammation it will too! Research suggests that omega 3 fatty acids that fight inflammation supporting vein health and elasticity, especially in a 6:1 ratio of EPA:DHA. [3]
A 2019 study also highlights the risk of fatty acid imbalance causing inflammation linked to vascular disease, "Epidemiological studies have shown that a lower EPA:AA ratio is associated with an increased risk of coronary artery disease, acute coronary syndrome, myocardial infarction, stroke, chronic heart failure, peripheral artery disease, and vascular disease." [4] *Note, the ratio is written as EPA:AA in this particular study, although fatty acid testing commonly flips it, calling it an AA:EPA ratio.
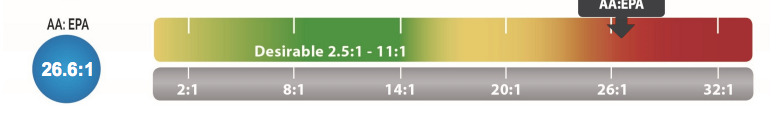
Find out if fatty acid imbalance is contributing to inflammation (via the AA:EPA ratio) and varicose veins with Fatty Acid Testing.
6) Work it (and not in high heels)
Varicose veins are especially common in the legs and calf, which can worsen with inactivity. Did you know that your movement in your heel and calf helps to pump the de-oxygenated blood up your legs back to your heart? This is drastically decreased when you wear high heeled shoes. If you work at a desk all day here are some of my favorite options to get you moving everyday: the treadmill desk and the treadmill laptop shelf.
7) Compression stockings
One of the first thing a vascular specialist might do is give you a Rx for a custom sized compression stocking to wear during the day to help provide support, and to force blood to circulate through the deeper veins instead of the surface veins that are commonly problematic. Wearing these can help slow the progression of varicose veins, according to Western medicine. However, they are not particularly cheap, usually costing around $100-$130 per pair.
8) Address Hypercoagulation
If your blood is thick and sticky from hypercoagulation, those vein valves have to do a lot more work.
Blood health and homeostasis are rarely talked about until there's a big problem (read: you get a blood clot), so you probably haven't heard much about hypercoagulation.
If you were to take all the blood vessels out of an adult body (talking about arteries, veins, capillaries) and lay them out in a straight line, it would end up spanning a length of approximately 100,000 miles.
This is the highway for your immune system as well as for your body to deliver oxygen, nutrients, and hormones to cells as well as remove waste products.
What if your circulation highway is more like a 5'clock traffic jam due to thick, sticky blood slowing down the flow of 'traffic' in your bloodstream?
The impact on your veins isn't going to be great.
Find out what you can do to support blood health here.
Need extra help?
So while I've yet to see varicose veins vanish, I have seen vein pain disappear and varicose vein progression improve with nutrition. Why not make sure that you are supporting your veins with nutrition, and set the stage for what your body needs for your veins to work properly?
Learn more in the Align to Detox masterclass, request a free 15 minute consultation, or consider a one-on-one consultation with hair analysis and blood labs testing.
So tell me, what do you think?
References:
1. Peat, Raymond. Bleeding, clotting, cancer. 2006. Retrieved September 24, 2013, from http://raypeat.com/articles/aging/bleeding-clotting-cancer.shtml
2. Weatherby, Dicken. Signs and Symptoms Analysis from a Functional Perspective. Nutritional Therapy Association, 2004. Print.
3. https://www.mdpi.com/1422-0067/21/3/920/pdf
4. https://www.tandfonline.com/doi/full/10.1080/00325481.2019.1607414
5. Wikipedia. Varicose Veins. 2013. Retrieved September 24, 2013, from http://en.wikipedia.org/wiki/Varicose_veins






TeaJae says
so glad you put this up, I thought they were apart of life and at a certain ages you get them. The body can repair itself if you give it what it needs. Thank you for this 🙂
Kim says
As a Vascular Technologist, I diagnose valvular incompetence, or venous reflux on a daily basis. A great, and research proven, natural "remedy" for pain caused by varicose veins (caused by venous reflux) is to wear compression stockings consistently. Otherwise they will likely get worse, no matter how healthy you are eating! I'm surprised this artcle makes no mention of compression therapy for the treatment of varicose veins, as it is natural, safe and effective!
Bri says
probably because there merely a band-aide and don't fix the problem not to mention there very uncomfortable to wear and more visually distracting than varicose veins themselves. As a temporary solution its acceptable but should never be considered a long-term solution. Imagine wearing a big uncomfortable band-aide the rest of your life and that's why you don't see very many people wearing them
Vita @ VitaLivesFree says
Very true! My husband has had them all his life and since we went Paleo, his varicose veins have nearly disappeared. Diet and lifestyle can really change so many things.
Carl says
How long has your husband had these veins? I am 50 lbs. overweight and have had the veins for about 15 yrs. We are going Paleo for health reasons and was curious about abything you could tell me.
Thanks
Fera says
I have varicose veins running in my family. My mom has it, my aunts have it, by grandparents have it. I have read a study about how in Africa there is virtually no cases of people having varicose veins, Diabetes and heart diseases. Their diet is lacking all animal products or if they do have it (which is very rarely) it is used for flavoring. I have decided to try it! I have been a vegetarian for 7-8 years and mostly vegan for about 2 years. My mom at my age had already a very bad case of varicose veins where it was so painful that she had to go through surgery. Her calves looked so scary that she always had to wear pants. Poor thing, she was self conscious about them all her life. Although I have no varicose veins, I still feel that I have it in my genes because my legs tend to get tired a lot and I do feel heaviness sometimes at the end of the day (especially my calves). But I also know that we have a power to control those genes by diet and keep it in check. Please try plant based diet and no processed foods. Incorporate a lot of dark leafy green vegetables. You will not only feel the difference with your veins but you will also notice the difference in your health overall! Good luck!!
Stephen says
I'm Stephen from Uganda: these veins have started itching me,can they still cure? And by what methods? Thanks for your response please
Claire says
This is soooo encouraging. I'm paleo and hope my disappear.
Wendy says
Whats the name of the compression stockings he wore
Emily says
I've had them since I was about 13. I've never been overweight but they run in my family. After I had my son, they were horrible. They got huge and throbbed all day long. So I made an appt with a vein specialist. I had sclerotherapy done and OMG it was heaven. Talk about instant relief. I need it done again but it's pretty pricy. I am also hypothyroid and have a new nodule on my thyroid. I am a newbie at gluten-free and I am pleasantly surprised to see that it could help with my nasty veins too!
Letty says
Interesting article/post! Any recommendations on the related condition of lipedema? It's very under diagnosed but I have heard diet can really have an affect there as well!.
Love to hear your thoughts.
nancy crawford says
Please don't scare people away from "expensive" compression stockings/socks. There are many out there available in moderate to heavy compression (ie 15-20mmgh or 20-30mmgh) for well under $100. I own about 15 pair and wear them daily to work, when I run (scrunched down so as not to look like a hillbilly - lol) and just running errands. These are not your grandmother's compression stockings. I don't have a problem w/ my veins and hope to keep it this way.
Petunia53 says
Nancy Crawford...I'm a bit confused about the "when I run....scrunched down so I don't look like a hillbilly" comment...does that mean you hide them while running? Don't you need them while running too? I'm just trying to figure out what you mean. I'd think they'd be beneficial to wear while running too, unless they fall down, I guess! LOL. Thanks for clearing this up for me! 🙂
Phan says
What is Paleo? Please explain.
chris says
Horse Chestnut has helped mine they are almost gone. So much relief!
Maartje says
do you take it intern of extern?
JT says
I have used HC too, for years, but there has been no change. What dose do you take daily? thanks!
sadaf asad says
this information is very good for us...in my case...its a begging of it....my mom has also the same problem...what should i do not to prolong it...ur advice vl b very informative for me...i hope u vl reply me soon..
Julie Rasmussen says
I am glad to see this post!
Kelly says
I have worked for a vascular surgeon for over 13 years, there are no nutritional supplements or pills that can make the varicose veins go away. Losing weight helps because you are not adding additional stress and pressure on your legs. Wearing compression stockings is a great way to reduce pain and heaviness of the legs. Some insurance companies will pay for them given the correct diagnosis code. Getting a venous ultrasound study that focuses on the saphenofemoral junction will help to determine if you have reflux. A simple in office procedure called an endovascular laser ablation can rid you of the excess pressure that is creating these varicose veins.
Again, there are ZERO pills/supplements that can fix the valves inside the veins (no mention of that throughout this article), BUT there are ways to get rid of them.
fon says
all due respect for your expertise in the surgical removal of vericose veins. You and your allopathic model of addressing the symptom and not the cause is completely innappropriate when speaking about nutritional causes and cures. you are in the surgery business. your Dr. got almost zero training on nutrition in medical school and just because he hasnt run across any Double blind studies in the New England Journal of Medicine in his spare time, doesnt mean he or you have any expertise at all, when it comes to causes and cures which are pretty much always caused by nutritional deficiencies. The lazy fallback answer is oh,its genetic, which is a bunch of b.s. when you consider that 90% of chronic conditions, including this one, didnt exist 100+ years ago.
Deepak Suri says
Hi,
Very well explained. Thanks for sharing.
Precaution is always better than cure. I am glad to know that it's not necessary you have to face varicose veins as you grow older, all matters taking care of it at the early age.
Becky says
I've had vericoise veins since I was 12. I've always eaten healthy and been active. They did get worse with my twin pregnancy. I now have thousands of spider veins, too. I've tried natural supplements and herbs but no change . I tried compression stockings but it only helped until I take them off. I've moved they are a bit better when I cut out sugar/alcohol. I probably had a wheat sensitivity as a kid. I do t eat gluten or dairy. I have eaten (and mostly eat) paleo but saw more changes when o addressed past candida issues. Still trying to find things that help and am considering getting them removed as I really do have thousands of spider veins in one of my feet. They no longer hurt and I don't have circulation issues, love your blog. Enjoyed this thread. Curious to keep learning.
Kelly says
That's a funny reply: "I've always eaten healthy"...and then four sentences later, "they are a bit better when I cut out sugar and alcohol." Sugar is the main culprit, and alcohol is a sugar.
ANA says
MY DAUGTHER HAS HER VEIN VERY BAD PLEASE TELL ME WHAT SHE CAN DO FOR HER VEIN WHAT IS PALEO
Katie says
How on earth are you supposed to “balance your hormones and get rid of excess estrogen”?
Jean says
I have had varicose veins since i was about 12 had my vein stripped 3 times injections stockings but I am elergic to the elastic makes my skin break out my legs gets so hot and itchy. REPLY
Ct says
Any thoughts about a relationship between nutrient deficiencies and DVT?